Quarterly insights: Healthcare technology
What PBM federal reform means for the Rx value chain

The business model that enabled three vertically integrated PBMs to control about 80% of all retail prescriptions in the United States is being fundamentally rewritten in the wake of the February passage of the Consolidated Appropriations Act of 2026. In its place, a new landscape is emerging defined by transparency, decisions driven by data, and the unbundling of pharmacy benefit services into specialized, technology-enabled components.
The legislation creates definable demand for transparency infrastructure, analytics, navigation tools and modern pharmacy benefit platforms. To organize the emerging competitive landscape, we map the post-reform prescription drug value chain across five functional categories – from how drugs are sourced and priced, to benefit adjudication and compliance infrastructure, to pharmacy analytics and dispensing technology at the point of care.
The companies highlighted in this report and in our market map represent a sampling of the emerging players positioned to benefit from these structural tailwinds.
TABLE OF CONTENTS
- A sea change in the pharmaceutical value chain
- The market structure under pressure
- What the 2026 CAA actually does
- State-level momentum
- Where the opportunity lives
- Benefit administration: Transparent PBMs find their moment
- Analytics and compliance: The new infrastructure layer
- Pharmacy network economics are being rewritten
- The M&A signal and what to watch
- Looking beyond the reckoning
- Healthcare tech indexes fall farther behind broader markets
- Healthcare IT M&A: Notable transactions include CirrusMD and Mytonomy
- Healthcare IT private placements: Notable transactions include Qualified Health and Thesis Care
A sea change in the pharmaceutical value chain
On Feb. 3, 2026, President Trump signed the Consolidated Appropriations Act of 2026, enacting the most comprehensive federal reform of pharmacy benefit managers (PBMs) in history. The legislation mandates 100% rebate pass-through to plan sponsors, unlinks PBM compensation from drug prices in favor of flat bona fide service fees, imposes semiannual transparency reporting requirements, and establishes “any willing pharmacy” network access provisions – all taking effect in 2028 and 2029.
This is not incremental reform. It is a structural repricing of the entire pharmaceutical value chain. The business model that enabled three vertically integrated PBMs to control approximately 80% of all retail prescriptions in the United States is being fundamentally rewritten. In its place, a new landscape is emerging defined by transparency, decisions by data, and the unbundling of pharmacy benefit services into specialized, technology-enabled components.
The implications extend well beyond the PBMs themselves. This reform touches every stakeholder in the healthcare ecosystem: plan sponsors who will, for the first time, have genuine visibility into their pharmacy economics; providers who prescribe at the point of care without knowing what a drug will cost the patient; pharmacies – particularly independent and community pharmacies – that have been squeezed by opaque reimbursement structures; and the emerging technology companies building the infrastructure to enable a more transparent, efficient prescription drug value chain.
The market structure under pressure
The U.S. pharmacy benefit management industry is one of the most concentrated sectors in American healthcare. A 2024 JAMA study found that CVS Caremark, Express Scripts (Cigna/Evernorth), and OptumRx (UnitedHealth Group) together account for approximately 74% of all retail prescriptions processed. Measured by the Herfindahl-Hirschman Index (HHI) – the standard metric the Department of Justice uses to evaluate market concentration – the overall PBM market scores 1,972, well above the threshold for a moderately concentrated market. Medicare Part D (drug coverage) is even more concentrated, scoring 2,399.
TABLE 1: PBM market concentration by payer segment
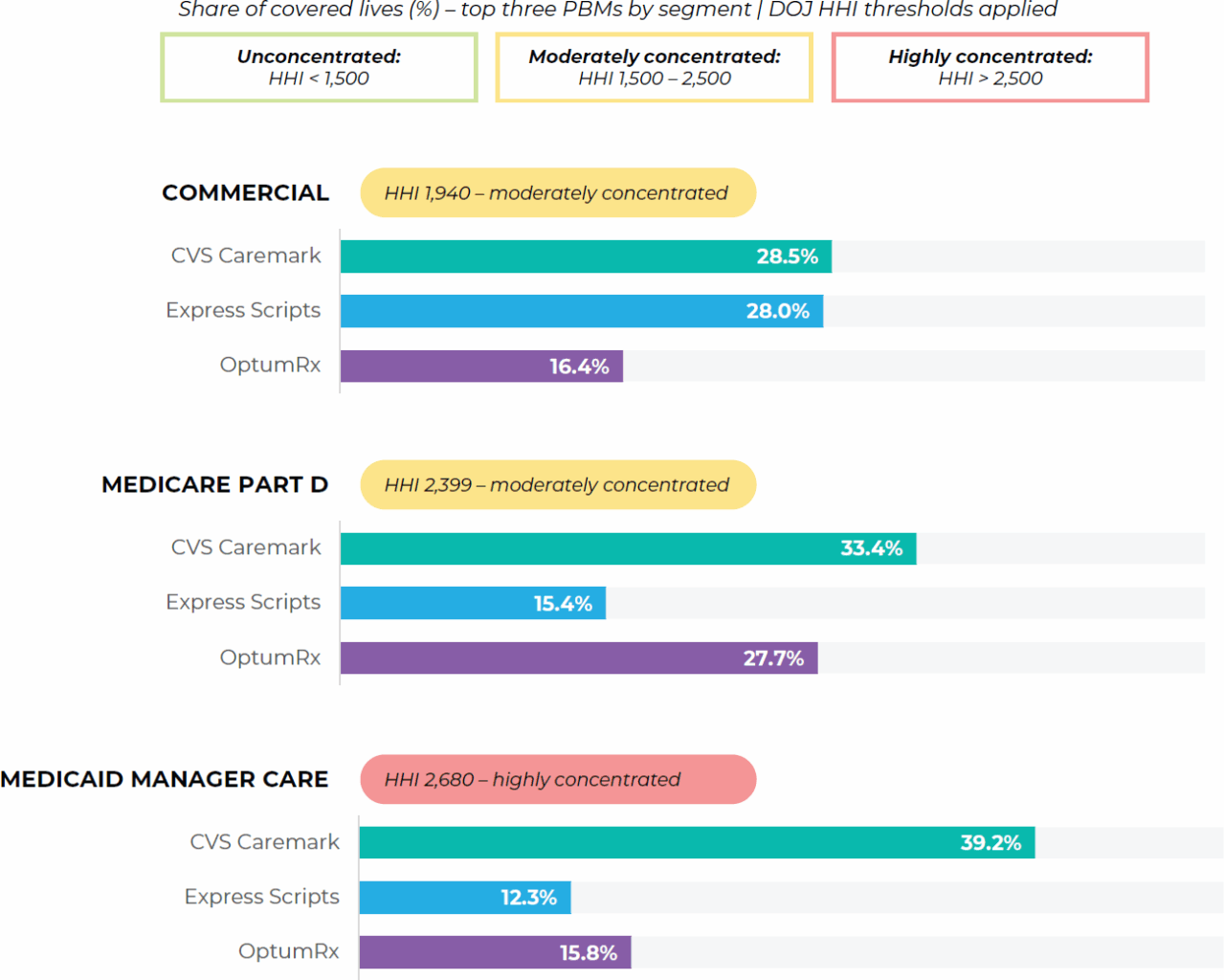
Source: Qato DM, Chen Y, Van Nuys K. Pharmacy Benefit Manager Market Concentration for Prescriptions Filled
at US Retail Pharmacies. JAMA. October 2024.
Critically, all three dominant PBMs sit inside vertically integrated parent companies that also own health insurers and pharmacy networks. CVS Health encompasses CVS Caremark, Aetna and the CVS retail pharmacy chain. Cigna’s Evernorth division includes Express Scripts and Accredo specialty pharmacy. UnitedHealth Group houses OptumRx alongside UnitedHealthcare and an expansive provider network. This vertical integration has drawn sustained scrutiny from the FTC, state attorneys general and bipartisan coalitions in Congress, who argue it creates inherent conflicts of interest, allowing PBMs to steer patients to affiliated pharmacies, favor higher-cost drugs with larger rebates, and retain economic value that should flow to plan sponsors and patients.
What the 2026 CAA actually does
The legislation addresses the PBM business model through four interlocking pillars.
First, beginning Jan. 1, 2028, PBMs under contract with Medicare Part D plan sponsors are prohibited from deriving remuneration from drug rebates, spread pricing or volume-based arrangements – an unlinking of compensation that breaks the economic incentive critics argue drives PBMs to prefer higher-list-price drugs with larger rebate structures.
Second, for commercial group health plans and plans governed under the Employee Retirement Income Security Act of 1974 (ERISA), PBMs must remit 100% of all rebates, fees and other remuneration received from manufacturers, group purchasing organizations, and rebate aggregators – quarterly, within 90 days – effectively eliminating spread pricing in the commercial market. This obligation took effect immediately upon enactment and extends ERISA’s definition of “covered service provider” to explicitly include PBMs, requiring disclosure of all direct and indirect compensation to plan fiduciaries.
Third, the legislation establishes a new transparency and audit framework. PBMs serving employer health plans must provide semiannual reports on net drug spending, rebates, spread pricing and benefit designs that steer utilization to affiliated pharmacies. Plan sponsors gain annual audit rights. Fourth, fines of up to $10,000 per day for information failures – and up to $100,000 for knowingly false submissions – give the reporting requirements real enforcement teeth. And effective Jan. 1, 2029, Part D sponsors must open their networks to any pharmacy meeting standard contract terms, with a new “essential retail pharmacy” designation protecting access in rural and underserved markets. The Department of Health and Human Services must define those contract terms by April 2028.
TABLE 2: Reform implementation timeline
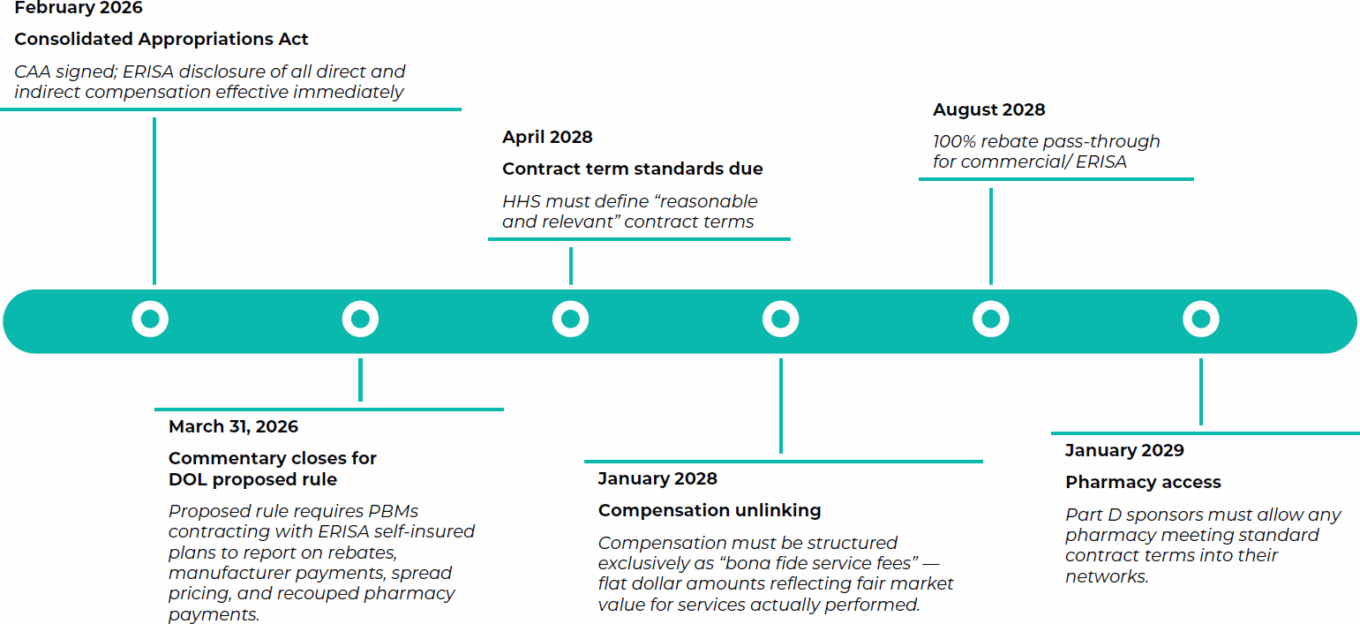
Source: First Analysis.
State-level momentum
Throughout 2025, states accelerated their own PBM reform efforts. Arkansas passed the first law banning PBM ownership of pharmacies, though a preliminary injunction has temporarily halted enforcement. Colorado and California enacted “delinking” laws prohibiting PBM compensation from being tied to drug prices. Massachusetts enacted comprehensive PBM licensing and transparency requirements. Utah and other states implemented rebate pass-through mandates. In April 2025, 39 state attorneys general signed a joint letter urging Congress to act.
In parallel, the Department of Labor issued a proposed rule on Jan. 29 requiring PBMs contracting with ERISA self-insured plans to report on rebates, manufacturer payments, spread pricing and recouped pharmacy payments. Comments closed March 31. This layered state, federal and regulatory activity creates a compliance environment that itself becomes a source of technology demand.
Where the opportunity lives
The reform does not simply constrain incumbents. It restructures competitive dynamics across the prescription drug value chain and creates demand for new capabilities at every layer.
TABLE 3: Surveyed employers’ primary PBM contracts, 2024 versus 2025
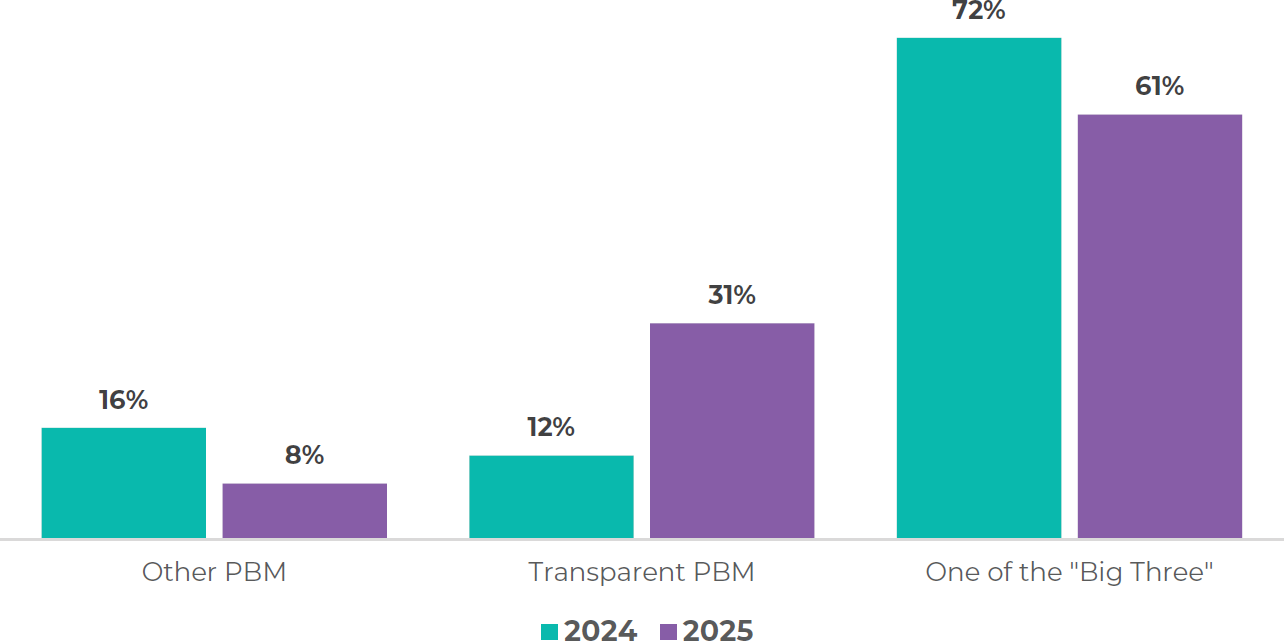
Source: National Alliance of Healthcare Purchaser Coalitions, 2025 Pulse of the Purchaser Survey, September
2025.
To organize the emerging competitive landscape, we map the post-reform prescription drug value chain across five functional categories – from how drugs are sourced and priced, to benefit adjudication and compliance infrastructure, to pharmacy analytics and dispensing technology at the point of care. The market map in Table 4 identifies a sampling of the companies building across this value chain, drawn from First Analysis’s proprietary company universe of more than 5,000 healthcare technology companies.
The flow follows the life cycle of a prescription dollar:
- Source: drug procurement and pricing
- Adjudicate: benefit administration and claims processing
- Verify: transparency, compliance and audit infrastructure
- Optimize: analytics, navigation and formulary intelligence
- Dispense: pharmacy network, electronic prescribing and medication management
TABLE 4: The prescription drug reform value chain – PBM market map
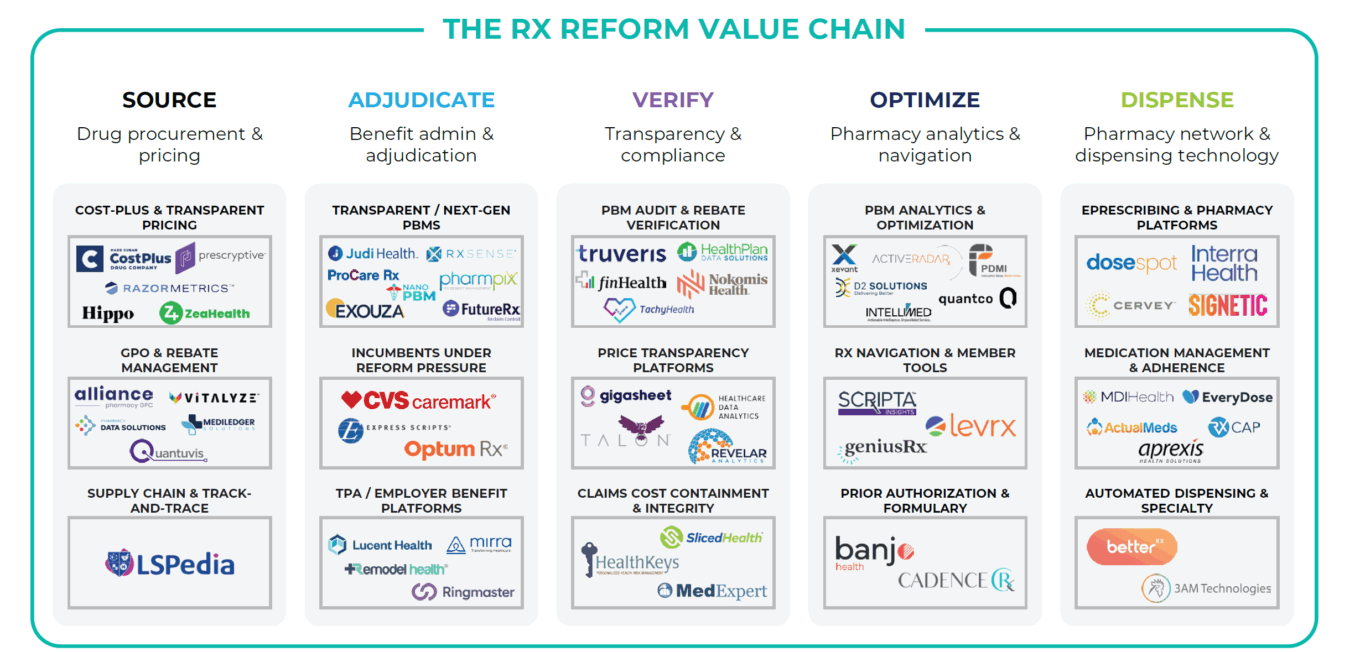
Source: First Analysis.
Each of the companies discussed in this report is positioned within one of these five categories. We highlight a subset below; the full market map provides a broader view of the competitive landscape.
Benefit administration: Transparent PBMs find their moment
The demand signal from employers was already moving before the legislation passed. A survey of 324 private and public employers and other healthcare purchasers indicated that between 2024 and 2025, employer adoption of alternative PBMs increased from 12% to 31%, while reliance on the three largest PBMs fell from 72% to 61%. The reform now effectively codifies the pass-through, flat-fee model as the industry standard by 2028, and employers have both the data and the regulatory framework to demand what they could previously only hope for.
Perhaps the most consequential market signal came from Blue Shield of California, which made the decision to unbundle its pharmacy benefit away from CVS Caremark entirely and rebuild it using a best-of-breed technology stack including Amazon Pharmacy and Mark Cuban Cost Plus Drugs – a move that demonstrated a major payer’s willingness to disaggregate the vertically integrated PBM model.
This shift is not limited to challenging the three vertically integrated incumbents. Established independent PBMs like Navitus (a transparent, 100% pass-through PBM owned by SSM Health), MedImpact (the largest privately held independent PBM), and Prime Therapeutics (the fourth-largest PBM, owned by a consortium of Blue Cross Blue Shield plans) are all navigating the reform environment from different strategic positions. Prime’s strategic alliance with Judi Health to migrate health plans onto the JUDI platform is a notable signal that even established PBMs see modern technology infrastructure as essential to competing in the post-reform landscape.
Among pure-play alternatives building market share now, three companies illustrate meaningfully different approaches to the same structural opening. Judi Health (formerly Capital Rx) has built an enterprise health platform that unifies pharmacy and medical claims adjudication under a flat-fee, 100% pass-through model. The scale is real: more than five million contracted employer PBM lives, with more than 80 new partnerships added in each of the past two years. Rightway takes a different route, pairing a transparent PBM with clinical care navigation – licensed pharmacists who guide members to lower-cost alternatives and manage the administrative friction of the pharmacy experience. It has won notable employer clients away from incumbents by demonstrating that transparency combined with navigation yields better outcomes than either alone. SmithRx, built on a modern in-house claims processing engine, targets the mid-market self-insured employer segment; its recent partnerships with agricultural and trade association health plans are a reminder that the transparent PBM wave extends well beyond large enterprises.
Analytics and compliance: The new infrastructure layer
Transparency generates data. The harder question is what happens next, because data without the tools to interpret and act on it is, for most employers, just noise. The new semiannual reporting requirements, audit rights and rebate pass-through tracking provisions create a new category of compliance-driven analytics demand. Employers who have never had visibility into their PBMs’ economics will need platforms to understand what they’re seeing. PBMs will need infrastructure to produce compliant reports and demonstrate value. Pharmacy navigation tools that surface lower-cost alternatives will become more valuable as cost transparency increases.
Truveris sits at the procurement end of this problem. Its Truveris Marketplace evaluates more than 60 PBMs and emerging providers, using historical claims data to predict what coverage an employer needs and enabling an apples-to-apples comparison that traditional broker-mediated requests for proposals cannot replicate. Ongoing claims analysis through its truGuard product monitors 100% of claims against PBM contracts to detect pricing variances, ensure compliance and satisfy fiduciary responsibilities – work that has helped employers save over $7 billion in cumulative pharmacy spend, including over $1.6 billion in savings for the state of New Jersey. In a post-reform world where plan sponsors gain audit rights and semiannual PBM reporting for the first time, the demand for independent procurement and oversight technology becomes structurally embedded.
The analytics layer runs deeper. Scripta Insights has built an AI-powered pharmacy navigation platform that sits alongside existing PBMs, providing transparency analytics and member-facing navigation tools for self-insured employers. Its proprietary Med Mapper engine analyzes over 17,000 medicines against payers’ benefit plans and PBM formularies to identify savings opportunities, and it generated 78,000 prescription switches in the past year with a 93% switch persistence rate after 12 months. Xevant addresses the same demand from the other direction: Rather than serving employers directly, it provides real-time, automated pharmacy benefit analytics for PBMs, third-party administrators, health plans and consultants, replacing manual report-building processes that traditionally took weeks. Its RebateLogic product automates managing and optimizing drug rebates, positioning Xevant as a “picks-and-shovels” play that serves both incumbent and disruptor PBMs navigating the new reporting environment.
The prior authorization workflow intersects with all of this. As one of the most friction-laden processes in the payer-provider relationship, the prior authorization workflow is being independently reshaped by the Centers for Medicare and Medicaid Services (CMS) prior authorization final rule and the Consolidated Appropriations Act’s transparency provisions. CoverMyMeds (McKesson) has built the dominant electronic prior authorization network, processing 43 million prior authorizations during the 2025 reverification season alone and connecting nearly a million providers with more than 50,000 pharmacies. Much of the underlying infrastructure runs through Surescripts, the nation’s leading health intelligence network, which processed 30.5 billion transactions in 2025 across electronic prescribing, benefit information, prior authorization and medication history. Surescripts’ Real-Time Prescription Benefit product, used more than one billion times by prescribers in 2025, is particularly relevant to the reform thesis, delivering the kind of point-of-care cost transparency the Consolidated Appropriations Act is working to mandate across the broader system.
For PBMs and health plans building or modernizing their benefit administration infrastructure, RxSense offers a different kind of leverage: It is not a PBM itself, but rather a cloud-based technology platform that PBMs, health plans and employers use to manage pharmacy benefits. Its RxIQ Enterprise platform cuts plan setup time in half, enables formulary updates in 30 minutes instead of weeks and uses AI and machine learning to price approximately 95% of its business in real time. The modular architecture serves both incumbents retrofitting for transparency and new entrants building from scratch.
Pharmacy network economics are being rewritten
The any-willing-pharmacy provisions and essential pharmacy designations that take effect in 2029 will do more than open networks. They will fundamentally change the economics of pharmacy distribution. Independent and community pharmacies gain new access and reimbursement protections. Specialty pharmacy distribution becomes more transparent. And the emergence of alternative pharmacy models – from Amazon Pharmacy’s RxPass subscription ($5 per month for common generics with home delivery) to GoodRx’s consumer discount platform connecting patients to lower-cost prescriptions across more than 70,000 pharmacies – creates competitive pressure on traditional distribution channels that the any-willing-pharmacy provisions will only intensify.
The most visible disruptor in the drug procurement and pricing layer has been the Mark Cuban Cost Plus Drug Company, which demonstrated early that a radically transparent pricing model – acquisition cost plus a 15% markup plus a flat dispensing fee, with more than 2,000 medications listed – resonates with both consumers and employers. The company has since expanded beyond direct-to-consumer mail order into employer and managed care organization channels, and it is building an affiliate network of independent community pharmacies that aligns directly with the Consolidated Appropriations Act’s network access provisions.
The M&A signal and what to watch
Early transaction activity suggests the PBM technology ecosystem is entering a period of accelerated consolidation, and two transactions illustrate the thesis. The recent formation of Interra Health through the merger of Arrive Health and DoseSpot with Bain Capital Tech Opportunities as majority owner validates that integrated prescription drug decision support and electronic prescribing infrastructure is consolidating into scaled, acquirable platforms. The combined company delivers real-time coverage, pricing and prior authorization insights at the point of prescribing. It is growing at approximately 40% annually and is profitable. Separately, Waltz Health, an AI-driven prescription pricing marketplace founded by former OptumRx/Catamaran CEO Mark Thierer, was acquired by EVERSANA in 2025 after building a platform that supported over 9 million patients and 80 million pharmacy transactions annually. As transparent PBM models scale and analytics companies demonstrate recurring revenue at the compliance layer, strategic acquirers and financial sponsors should continue to accelerate transaction activity across the sector.
While the reform has been enacted, several implementation milestones will determine how the competitive landscape ultimately shakes out. How CMS defines “reasonable and relevant” contract terms for the any-willing-pharmacy provisions will determine the practical economics of pharmacy network participation and independent pharmacy viability. (The defining rule is due by April 2028.) The Department of Labor’s final rule on ERISA PBM transparency will determine how disclosure obligations interact with and potentially extend beyond the Consolidated Appropriations Act’s legislative requirements. And the incumbent response from CVS Caremark, Express Scripts and OptumRx bears watching closely: All three have launched “transparent” pricing offerings in recent years, but whether these represent genuine restructuring or simply co-opt the transparency narrative will become apparent as the 2028 deadlines approach and employers can compare offerings against truly independent alternatives. Finally, the Consolidated Appropriations Act directs the Government Accountability Office to study price-based PBM compensation across Medicaid, laying groundwork for the next wave of reform in a market where CVS Caremark alone controls 39% of PBM services.
Looking beyond the reckoning
The PBM reckoning is not a single event. It is a multi-year restructuring of how America pays for prescription drugs. The legislation creates definable demand for transparency infrastructure, analytics, navigation tools and modern pharmacy benefit platforms. The companies highlighted in this report and in the accompanying market map represent a sampling of the emerging players positioned to benefit from these structural tailwinds. This list is not exhaustive, and the competitive landscape will continue to evolve as the 2028 and 2029 implementation dates approach.
What is clear is that the old model – opaque pricing, rebate-linked compensation, vertically integrated conflicts of interest – is being replaced by something more transparent, more technology-enabled and more aligned with the interests of the employers and patients who pay for prescription drugs. For investors, founders and operators in the healthcare technology ecosystem, this is one of the most significant structural opportunities in the sector today.
Healthcare tech indexes fall farther behind broader markets
The First Analysis Healthcare Technology Index finished the one-year period ended April 2 down 36% overall, with the payer technology subset down 45% and the provider technology subset down 32% versus the S&P 500’s 22% gain and Nasdaq’s 32% gain.
Of the 18 First Analysis healthcare technology stocks that were publicly traded at the beginning of the period, only two were up over the period. CareCloud (CCLD) increased by the most, 136%. The next largest gainer was Veradigm (MDRX), up 8%. Of the 16 stocks that declined, 13 declined by 20% or more. GoHealth (GOCO) declined the most, 89%, followed by eHealth (EHTH), which declined 81%. The largest detractors on a market-cap-weighted basis – Doximity (DOCS), down 61%, and Phreesia (PHR), down 68% – together accounted for well over half the index’s decline.
Healthcare technology public comparables*
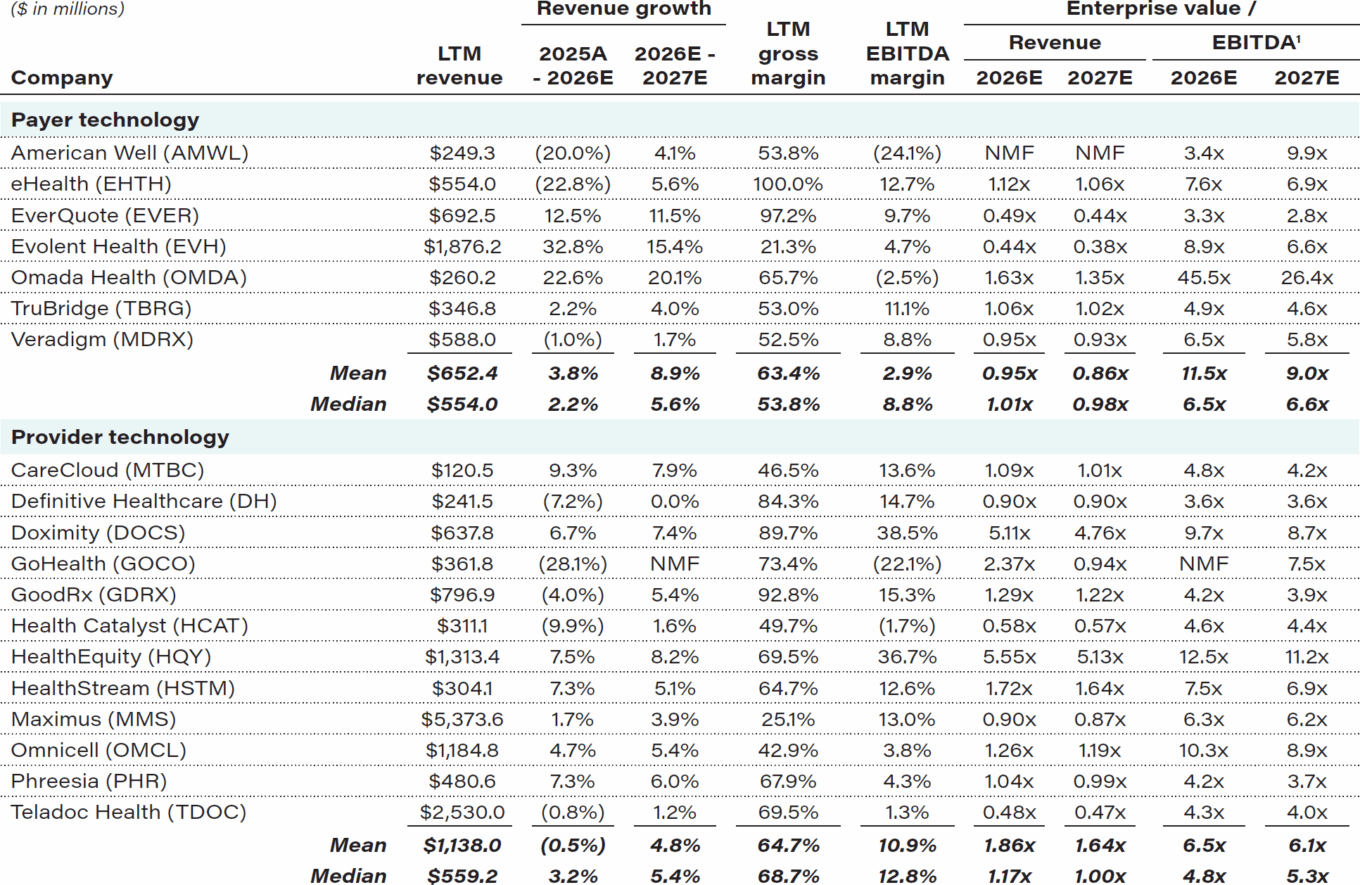
Source: Capital IQ, First Analysis.
Notes: Public comparable company data shown above is as of April 2, 2026. (1) EBITDA multiples less than 0 and greater than 50 labeled “not meaningful” (NMF). LTM = last 12 months. EBITDA = earnings before
interest, taxes, depreciation and amortization.
The indexes’ enterprise value multiples of trailing 12-month revenue as of April 2 were 0.73 for the payer technology subset and 1.63 for the provider technology subset. Regarding forward multiples, the average and median enterprise value multiples of 2026 estimated revenue were 0.9 and 1.0 for the payer technology subset and 1.9 and 1.2 for the provider technology subset. In the payer technology subset, Omada Health (OMDA) traded at the highest multiple of 2026 estimated revenue at 1.6, while HealthEquity (HQY) led the provider technology subset at 5.5. While revenue is expected to be about flat for both groups on average in 2026, it is expected to resume growing in 2027 (by 9% in the payer subset and by 5% in the provider subset).
First Analysis Healthcare Technology Index 1-year performance
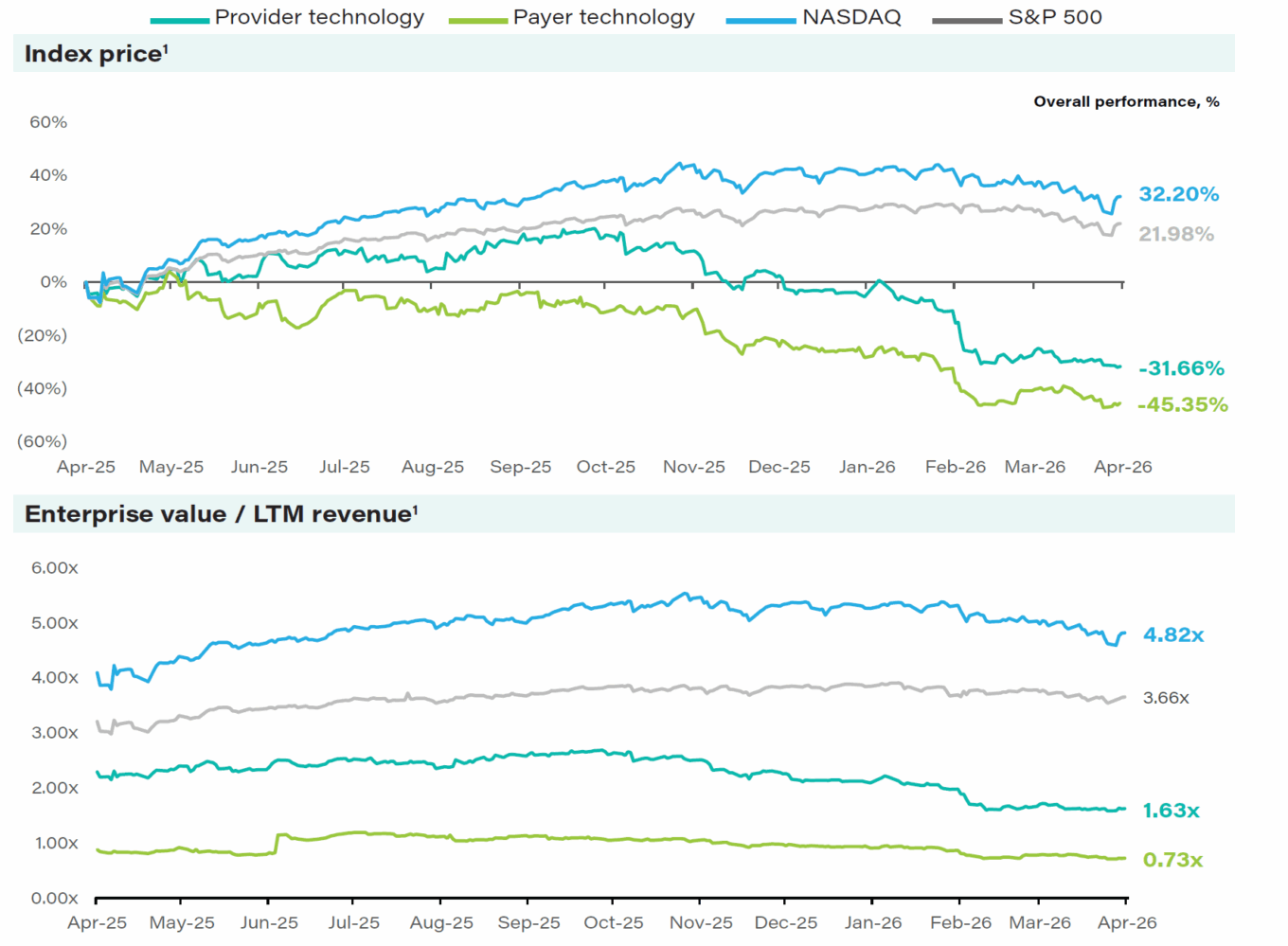
Source: Capital IQ.
Notes: (1) Index performance is based on market cap weighted constituents. For the period from April 2, 2025,
through April 2, 2026.
Healthcare IT M&A: Notable transactions include CirrusMD and Mytonomy
We highlight two noteworthy healthcare IT merger and acquisition announcements from the first quarter.
On March 3, Quantum Health announced it acquired CirrusMD, an on-demand virtual care company offering physician-led care around the clock every day. CirrusMD connects members with a doctor in under 60 seconds through chat-led care and provides comprehensive virtual primary care and urgent care services including annual wellness visits, weight management, women’s health, behavioral health support, lab orders and preventive screenings. Transaction terms were not disclosed.
Quantum Health is a healthcare navigation company specializing in identifying critical healthcare moments to enable early member engagement. The CirrusMD acquisition embeds physician-led virtual care into Quantum Health’s Real-Time Intercept model, strengthening the combined company’s ability to engage members at their first moment of need before care and costs escalate. The combined entity includes over 2,300 team members serving more than 20 million members across private and public sector organizations, positioning it to enable physician-driven referrals and proactive outreach that helps members avoid unnecessary emergency room visits.
CirrusMD’s generative AI solution WRITER offers patient-specific benefits recommendations to doctors in real time at the point of care
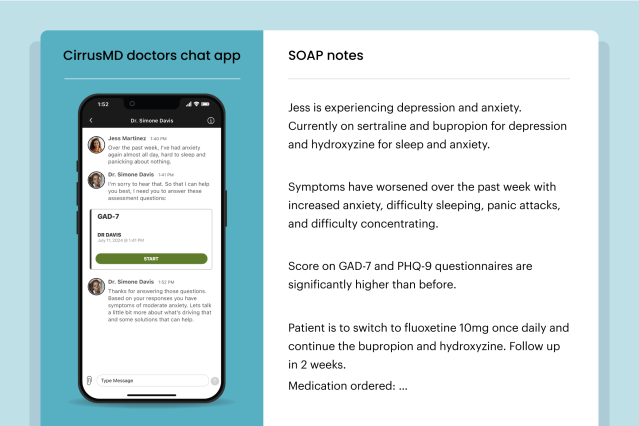
Source: CirrusMD.
On March 10, Elsevier announced an agreement to acquire Mytonomy, a leader in video-based patient engagement solutions. Mytonomy’s Cloud for Healthcare is a configurable enterprise SaaS platform that integrates clinically validated patient education videos, enterprise content management, survey tools and direct-to-patient communications within healthcare systems’ electronic health records (EHRs). The platform automates patient journeys within clinical workflows, driving personalized engagement and real-time analytics delivered within the patient portal and across multiple channels. Mytonomy is used at 70 hospitals and 200 clinics. Transaction terms were not disclosed.
Mytonomy Cloud for Healthcare automates patient journeys with clinically validated video education integrated into EHR workflows
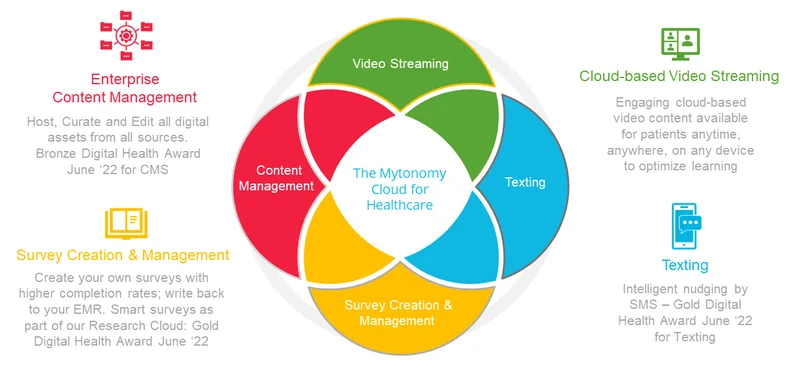
Source: Mytonomy.
The acquisition complements Elsevier’s Clinical Solutions portfolio, which includes PatientPass, ClinicalKey AI and ClinicalSkills. Combining the two strengthens Elsevier’s patient engagement capabilities with standardized written and multimedia education integrated into EHR workflows. The acquisition positions the combined companies to enhance outcomes while supporting Elsevier’s broader clinical intelligence capabilities. For example, surgery patients in treatment pathways covered under the Centers for Medicare and Medicaid Services watch over 20 minutes per session, and 73% of patients surveyed said Mytonomy video viewing helped them adhere to their care plans.
Select recent M&A transactions (sorted by date of announcement)
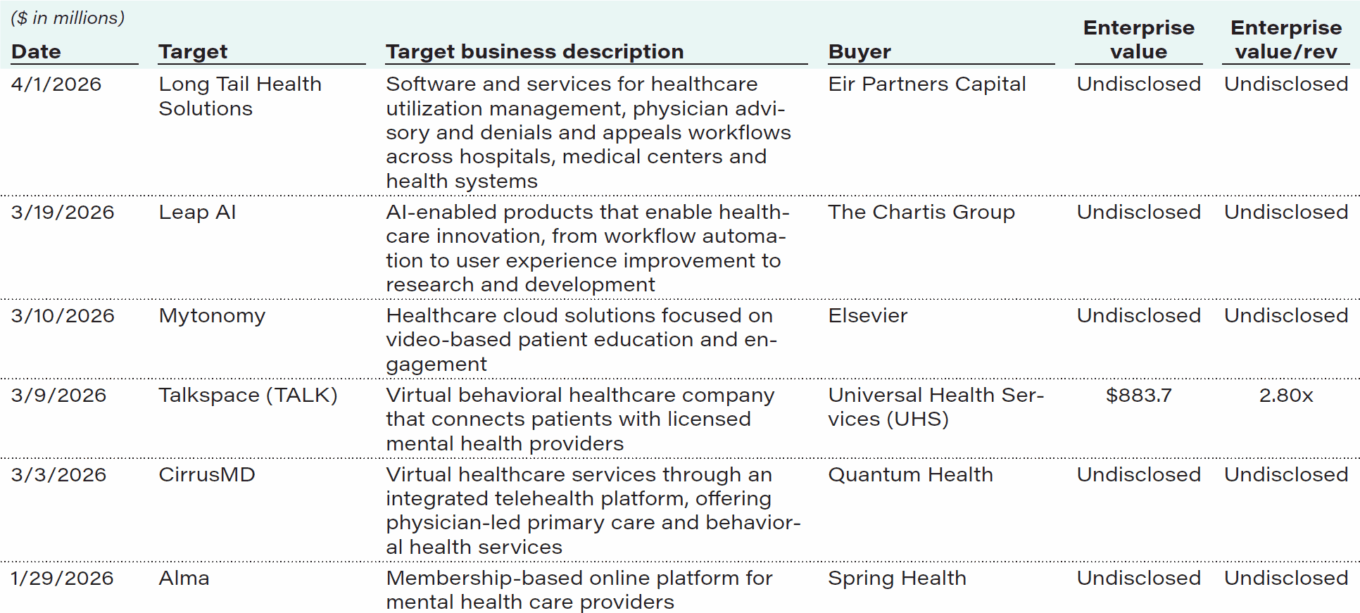
Source: Capital IQ, First Analysis.
Healthcare IT private placements: Notable transactions include Qualified Health and Thesis Care
We highlight two noteworthy healthcare IT private placement announcements from the first quarter.
In late March, Qualified Health announced a $125 million Series B funding led by New Enterprise Associates with participation from Transformation Capital, GreatPoint Ventures, Cathay Innovation, Anthropic and Menlo Ventures’ Anthology fund, along with existing investors SignalFire, Frist Cressey Ventures, Flare Capital Partners, Healthier Capital, Town Hall Ventures, and Intermountain Ventures. Founded in 2023, Qualified Health offers health systems an enterprise-wide AI platform designed to promote safe and responsible AI integration.
Qualified Health’s enterprise AI platform embeds safety, governance and clinician oversight across health system workflows
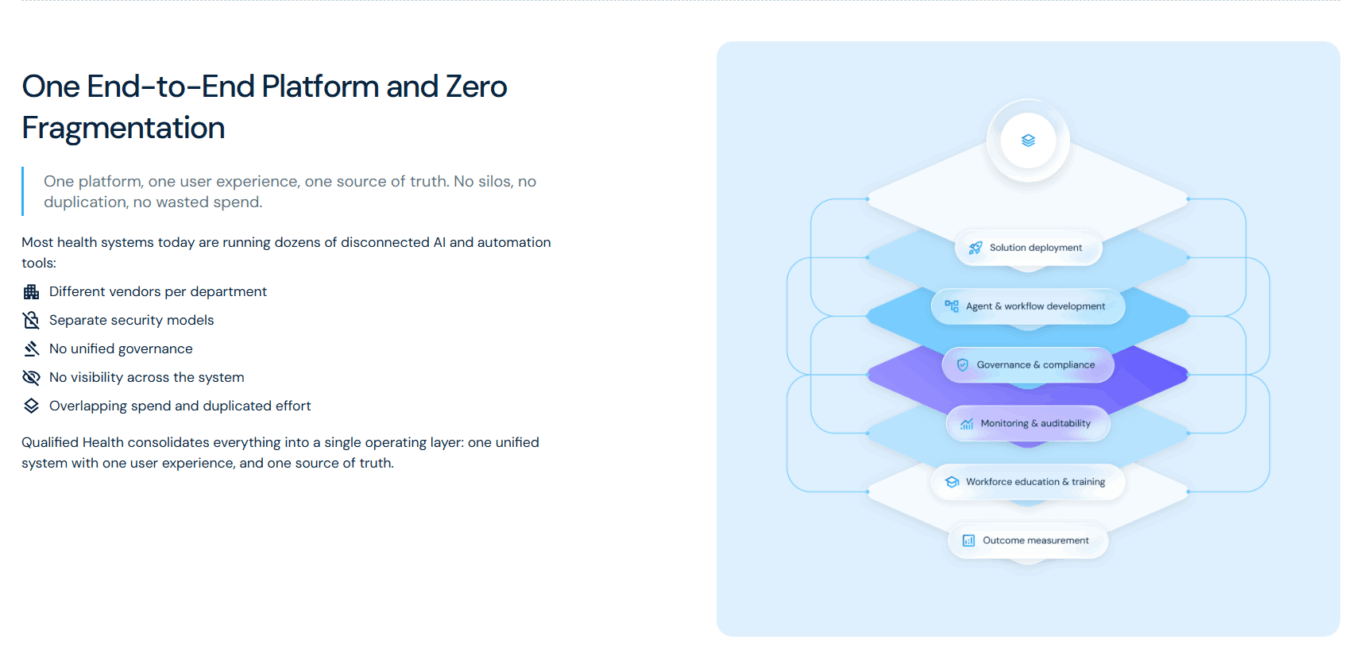
Source: Qualified Health.
The platform embeds safety and governance including clinician oversight, full auditability, source attributions and continuous monitoring. Qualified Health supports 400,000 users representing approximately 5% of U.S. hospital revenue, with partners including Emory Healthcare, University of Rochester Medicine, Jefferson Health and all eight health institutions of the University of Texas System. At University of Texas Medical Branch, Qualified Health generated more than $15 million in measurable run-rate impact within the first six months. The company plans to use the Series B funding to deepen relationships with existing partners, expand its U.S. hospital footprint, and invest in product development and engineering. The transaction underscores investor confidence in AI governance solutions as healthcare systems seek to accelerate clinical AI adoption while managing safety and compliance risks.
On March 25, Thesis Care (formerly Trovo Health) announced a $45 million Series A funding led by Oak HC/FT with participation from CRV and Black Opal Ventures. The round brings total funding to $60 million. Thesis Care is an AI-powered care team platform for scalable clinical capacity that deploys AI agents backed by expert clinicians to take on high-impact clinical operations and care management work for healthcare organizations. The platform is powered by AI that understands clinical context to deliver personalized patient engagement and complete workflow actions while knowing when to engage Thesis Care’s team of clinical experts, completing tasks end-to-end without requiring staff to learn a new tool.
Thesis Care deploys AI agents backed by expert clinicians to deliver scalable clinical capacity
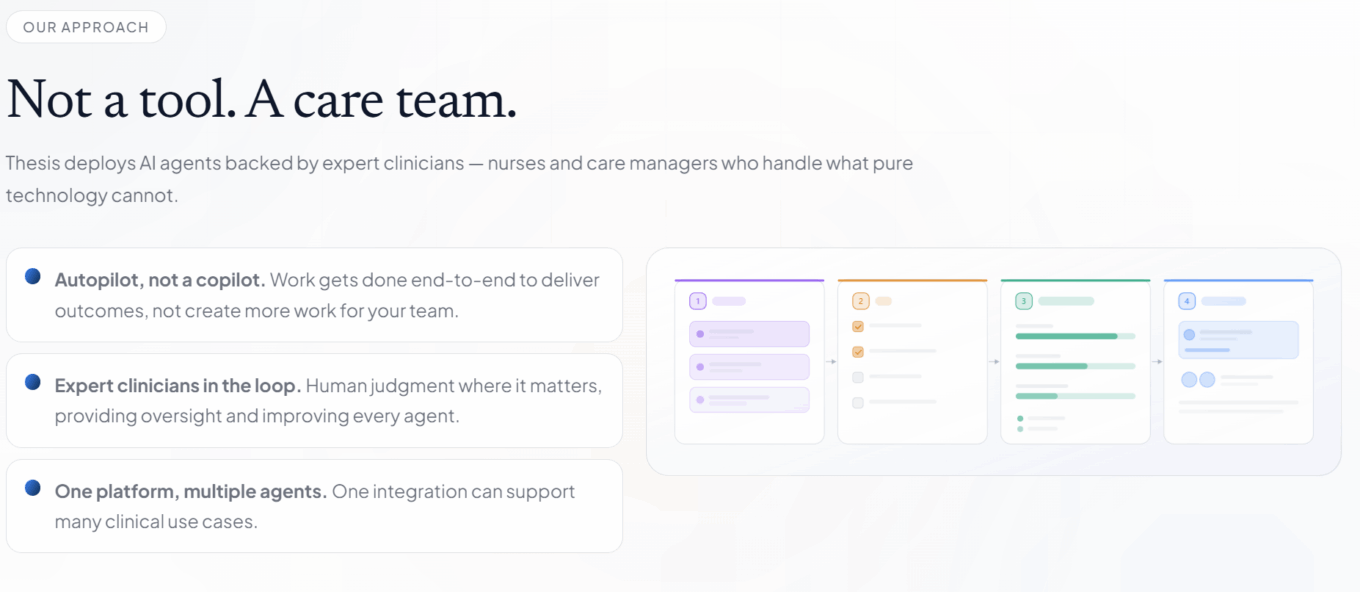
Source: Thesis Care.
Founded in 2024 by Niren Gandra and Aditya Pandyaram, Thesis Care has partnerships covering thousands of providers including US Heart & Vascular, Essen Health Care, Springfield Clinic, Unio Health Partners and Allied Digestive Health, with expansion underway into health systems and health plan care teams. The funding will be used to accelerate commercial expansion, deepen the unified technology platform, and broaden its suite of care team agents. This transaction exemplifies investor appetite for AI-augmented clinical operations that combine automation with human clinician expertise to improve care efficiency and quality outcomes.
Select recent private placements (sorted by date of announcement)
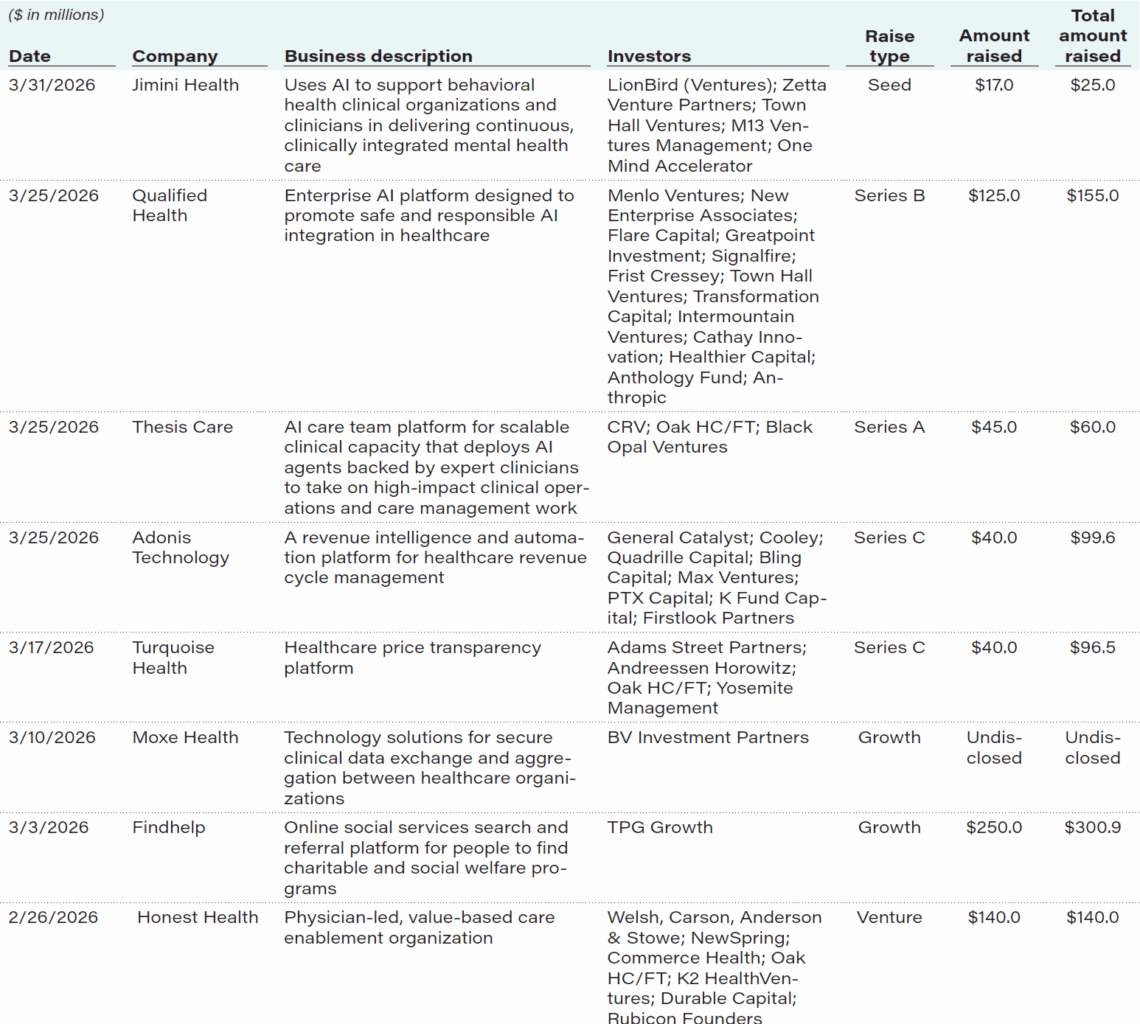
Source: Capital IQ, First Analysis.

Request full report
To access the full report, please provide your contact information in the form below. Thank you for your interest in First Analysis research.
