Quarterly insights: Healthcare technology
How healthcare is finally learning to use the data it has

The healthcare system has enormous amounts of valuable data. The problem is that data doesn’t move to the right place, at the right time, and in a form that providers and others can act on.
The failure of clinical data to reach the point of care is not merely an operational inconvenience. It has measurable, substantial financial and clinical consequences.
Challenges to realizing the full value of healthcare data include the diverse range of care settings where it must be delivered, the often messy, unstructured nature of clinical data, and the privacy sensitivity of clinical data, which requires extensive governance architectures.
The ongoing transition from systems of record to systems of action is a layered progression of capabilities. We map those layers across the four eras of clinical data infrastructure and show why the exchange and transport layer running through all of them only grows in strategic importance as the application layers above it become more sophisticated.
We profile a sample of companies building solutions in this space and provide a framework for evaluating them.
TABLE OF CONTENTS
- The data paradox
- Other sectors have already addressed this paradox
- The evolution of clinical data exchange
- What fragmentation actually costs
- Challenges on the path to delivery
- The infrastructure stack and where value is being created
- Where the opportunity is taking shape
- A sampling of companies building in this space
- Evaluating the category
- The transition underway
- Sector market activity: Healthcare tech index performance, M&A activity highlighting Knack RCM, EqualizeRCM and Bonsai Health, and private placement activity highlighting Enzo Health and Luminai .
Includes profiles of Abridge, Arcadia, Bamboo Health, Episource, Hart, IMO Health, Inovalon, Iodine, Kno2, Mede Analytics, Metriport, Moxe Health, Navina, Nym Health, Redox, Rhapsody, Surescripts, Tennr, Veradigm, Verato, Vim
The data paradox
Consider what happens when a patient with congestive heart failure, Type 2 diabetes, and a recent behavioral health hospitalization is discharged from a skilled nursing facility and admitted to a home health program. The receiving home health nurse needs to know—right now, at the kitchen table on day one—what medications were changed at the skilled nursing facility, what the cardiologist noted at the last visit, and whether there are active behavioral health concerns that affect care planning.
That information almost certainly exists somewhere. It was documented, coded and stored. But the odds that it arrives at that kitchen table, in a form the nurse can use, and at the moment it is needed are not good. It might arrive as a 47-page PDF discharge summary, if it arrives at all. Most likely it arrives days later, after the nurse has already made clinical decisions without it.
This is the central paradox of American healthcare data: The United States has built the most extensively documented healthcare system in human history, and it still routinely makes care decisions in the dark.
The problem is that data doesn’t move to the right place, at the right time, and in a form that anyone can act on. For two decades, the healthcare industry has labored to solve what it called an interoperability problem. But it’s actually a more fundamental challenge: the difference between systems that store information and systems that deliver it where it can do some good. This distinction between systems of record and systems of action is reshaping how sophisticated health plans, providers and technology investors think about clinical data infrastructure. And understanding it is the key to understanding where the next era of healthcare value is being created.
The United States has built the most extensively documented healthcare system in human history, and it still routinely makes care decisions in the dark.
Other sectors have already addressed this paradox
Healthcare is not the first industry to discover that storing information and delivering it are entirely different problems. Other sectors solved this gap a decade ago, and the companies that built the delivery layer captured most of the value. Salesforce didn’t replace the contact database. It built a layer on top of it that surfaced the right information at the right moment in the sales workflow, such as a prompt before a call, an alert when a deal went cold, or a recommendation before a renewal. The record became the foundation for action. The companies that owned the action layer captured the market. Workday and ServiceNow did the same thing in human capital management. In financial services and supply chain, value migrated the same direction, from the systems that stored information to the systems that delivered it inside the workflow where someone needed to act on it. The systems of record became table stakes. The action layer became the business.
Healthcare is arriving at this transition about a decade late. The stakes are different. They are measured not in lost deals or supply chain inefficiencies but in clinical outcomes and patient safety.
The electronic health record (EHR) is healthcare’s system of record. It is an extraordinarily capable tool for documenting clinical encounters, supporting billing and coding, and maintaining longitudinal patient records. The EHR does well what it was built to do. The mistake has been expecting it to do something it was never designed for: deliver discrete, actionable clinical intelligence at the point of care, in real time, across the fragmented ecosystem of settings where patients receive care. That is a different capability entirely, and it is the capability that the next generation of healthcare infrastructure is being built to provide.
The evolution of clinical data exchange
The history of clinical data exchange falls into three distinct eras, each representing a meaningful advance over what came before and each revealing the limits of what the previous approach could deliver. A fourth era lies ahead.
Getting data into systems (2009–2018)
The Health Information Technology for Economic and Clinical Health Act (HITECH), passed as part of the 2009 stimulus package, set off the most rapid technology adoption in the history of American medicine. Hospital EHR adoption went from roughly 10% to more than 80% within a decade. Medical records that had lived in paper charts moved into digital systems.
This was real progress. But the mandate optimized for a specific outcome: digitization. The goal was to get data into systems of record, not to make it flow between them. By 2015, the United States had accumulated an unprecedented volume of digital clinical data, locked inside thousands of siloed EHR installations from dozens of vendors, none of which were designed to communicate with each other.
The exchange mechanisms that existed in this era were primarily designed to move files between systems. A document created with the Consolidated Clinical Document Architecture (C-CDA) standard could technically transmit a patient’s clinical history from one system to another. But in practice, these were dense, difficult-to-parse documents that often ran dozens of pages. It was like attaching a filing cabinet to an email: The information was there, but it wasn’t usable. This first era effectively built better filing cabinets and called it interoperability. The data was stored. It was rarely delivered.
The exchange mechanisms … could technically transmit a patient’s clinical history from one system to another. But in practice, these were dense, difficult-to-parse documents that often ran dozens of pages. The information was there, but it wasn’t usable. This first era effectively built better filing cabinets and called it interoperability. The data was stored. It was rarely delivered.
Getting systems to talk (2018–present)
The 21st Century Cures Act, enacted in 2016 and implemented over the following years, represented a fundamental shift in the regulatory approach to healthcare data. Where HITECH had incentivized digitization, the Cures Act attacked the structural barriers to exchange, requiring the adoption of standardized Fast Healthcare Interoperability Resources (FHIR) application programming interfaces (APIs) and explicitly prohibiting information blocking by providers, health systems and health IT developers.
FHIR was a genuine technical advance. Unlike its predecessors, FHIR is built on the same architectural principles as the modern web: a resource-based data model that allows discrete data elements to be queried individually rather than bundled into unwieldy documents. The Trusted Exchange Framework and Common Agreement (TEFCA) established a national exchange architecture, and a set of Qualified Health Information Networks served as the backbone for nationwide data sharing. Da Vinci Project use cases defined specific FHIR-based workflows for prior authorization, coverage requirements discovery and payer-to-payer data transfer.
This was significant progress. But this second era, for all its advances, remains primarily an infrastructure of connections between major stakeholders. It has not solved the problem of getting discrete, actionable clinical data to the diverse array of settings where care happens, such as home health agencies, skilled nursing facilities, behavioral health providers, and community health workers who make home visits. A FHIR API that a developer can query is not a system of action. It is a more sophisticated system of record with better access controls.
Getting data to where it can do something (emerging now)
The defining question of the third era is not “can systems talk to each other?” The question now is whether the right discrete piece of clinical information, such as a medication change, an active diagnosis, a pending care gap, or a recent hospitalization, can be delivered automatically to the right person at the right moment, embedded in the workflow where they will actually use it, regardless of where care is happening.
That is a fundamentally different capability from what previous eras were built to provide. It requires not just exchange infrastructure but normalization, intelligence and delivery. It means turning raw data into structured facts, routing those facts to the appropriate endpoint, and surfacing them in a form that can drive clinical action without adding burden to the care team. This is the systems-of-action layer, and it is being built now.
Getting out of the way entirely (on the horizon)
A fourth era is taking shape on the horizon, one that may ultimately render the distinction between data delivery and clinical action moot. As AI foundation models trained on clinical data mature and as AI agents become capable of querying exchange networks, interpreting results, and acting on them autonomously, the systems-of-action layer begins to collapse into something more fundamental: infrastructure that doesn’t just surface the right fact at the right moment, but responds to it. The implications for clinical governance, regulatory oversight, and data permission management are not yet defined, but they will soon need to be. Nonetheless, it’s clear today that the exchange and transport infrastructure being built now will be strategically important well beyond the current regulatory cycle. The pipes that the fourth era will run on are being laid in the third era.
As AI foundation models trained on clinical data mature, the systems-of-action layer begins to collapse into something more fundamental: infrastructure that doesn’t just surface the right fact at the right moment, but also responds to it.
What fragmentation actually costs
The failure of clinical data to reach the point of care has measurable, substantial financial and clinical consequences, so organizations that solve the problem can offer concrete return on investment.
Risk adjustment and HCC capture
Medicare Advantage plans are reimbursed based in part on the documented health status of their members, a process that relies on Hierarchical Condition Category (HCC) coding derived from clinical encounters. When a member’s chronic conditions are not documented in the claims data because the relevant clinical evidence never made it into the payer’s systems, the plan is reimbursed as if that member is healthier than they are. The result is risk adjustment leakage: plans systematically under-capturing the revenue they are entitled to for the complexity of their members. The traditional remedy—retrospective chart review—is expensive, incomplete and increasingly insufficient as Medicare Advantage margins compress. Prospective and concurrent capture of HCC-relevant clinical evidence, surfaced at the point of care, is the more effective and durable solution.
Quality gap closure
HEDIS measures, the standardized quality metrics that determine star ratings for Medicare Advantage plans and drive significant bonus payment eligibility, are substantially driven by whether preventive and chronic care services are documented as completed. A significant portion of open quality gaps represent care that has actually been provided but never documented in a way that reaches the plan’s quality tracking systems. Without exchange infrastructure that reaches diverse care settings, the gap remains open and star ratings suffer regardless of whether the care was actually delivered.
Prior authorization burden
The prior authorization process is perhaps the most visible manifestation of clinical data fragmentation. Decisions that should take hours take days or weeks; staff on both sides spend time on administrative back-and-forth that adds no clinical value. The Centers for Medicare & Medicaid Services’ (CMS) Interoperability and Prior Authorization Final Rule, finalized in 2024 and implementing major provisions in 2026 and 2027, mandates that large payers implement FHIR-based prior authorization APIs. Plans that have invested in systems-of-action infrastructure are positioned to comply efficiently; those that haven’t face substantial operational and technology lift.
Care transitions: The highest-risk moment
Transitions between care settings are consistently the highest-risk moments in patients’ care journeys. An admission, discharge, and transfer (ADT) notification tells the receiving care team that a patient has moved. It does not tell them what medications were changed, what the clinical status was at discharge, or what the patient’s behavioral health situation looks like. The notification is a signal without content. The systems-of-action opportunity is to make that signal carry the clinical context that makes it actionable, transforming a data point into a care prompt.
Challenges on the path to delivery
The language of healthcare interoperability has always centered on exchange: data moving from one place to another, systems connecting to systems, networks enabling access. This framing is not wrong, but it has consistently obscured the harder and more important problem.
A relevant analogy is that the insight that drove the CRM category wasn’t that sales teams needed better databases. It was that the right information needed to arrive in the salesperson’s workflow at the right moment, without requiring them to know where to look for it. Healthcare needs the same transition: not data as a document to be read, but as a fact to be acted on.
The “wherever care happens” problem
Large hospital systems and major physician enterprises have invested heavily in EHR infrastructure. Their data challenges are real, but they have a foundation. In contrast, home health agencies, skilled nursing facilities, behavioral health providers, community-based organizations and independent specialty practices often lack that foundation entirely. These are the settings where the highest-risk, highest-cost patients, such as dual eligible members, complex chronic patients and individuals with behavioral health comorbidities receive substantial portions of their care. The data gap at these nodes is where the most harm occurs and where the most unnecessary cost accumulates.
Home health agencies, skilled nursing facilities, behavioral health providers, community-based organizations and independent specialty practices … are the settings where the highest-risk, highest-cost patients … receive substantial portions of their care. The data gap at these nodes is where the most harm occurs and where the most unnecessary cost accumulates.
Particularly for dual eligible beneficiaries (individuals who qualify for both Medicare and Medicaid and who account for a disproportionate share of total program spending), the fragmentation of data across multiple payers, care settings and regulatory frameworks creates a compounding problem at every transition. Each handoff is a potential data failure, and these patients have more handoffs than any other population.
Discrete data versus documents: Why it matters
A C-CDA discharge summary contains, somewhere within its dozens of pages, the patient’s active medication list. Finding it, parsing it and confirming its accuracy requires a trained clinician with time, a resource in perpetually short supply at the point of care. A structured FHIR Medication resource, delivered directly to a home health application at the moment of a first visit, presents the medication list in a clean, standardized format that can be reviewed, reconciled and acted on in minutes.
Making this work at scale requires normalization infrastructure that can extract structured data elements from the inconsistent, often messy real-world clinical data that flows through exchange networks. It requires natural language processing and AI capabilities that can convert unstructured clinical text into discrete facts that can be queried. And it requires delivery infrastructure that can route those facts to the right endpoint at the right moment without requiring clinical staff to initiate the query.
Governance as architecture, not afterthought
As clinical data exchange becomes more targeted and granular, the framework governing that exchange must become correspondingly more sophisticated. This is a design requirement for realizing the systems-of-action opportunity. Organizations that treat governance as a compliance checkbox will build systems that clinicians and patients don’t trust. Organizations that embed governance into their delivery architecture will build systems that get adopted, used and scaled.
The framework governing clinical data exchange must become correspondingly more sophisticated … organizations that embed governance into their delivery architecture will build systems that get adopted, used and scaled.
The HIPAA framework: Treatment, payment, and operations
The Health Insurance Portability and Accountability Act (HIPAA) Privacy Rule establishes the permissible purposes for which protected health information can be used and disclosed: treatment, payment and operations (TPO). As data delivery becomes more targeted and discrete, the logic for granting permissions must become more precise. A medication history provided to a home health nurse treating a patient is a treatment disclosure. The same data provided to a utilization management reviewer is a payment disclosure, and the same data provided to a population health analyst is an operations disclosure. Each carries different access parameters. Well-designed systems of action implement this logic in real time by embedding permissioning in the delivery architecture.
The hardest case: Behavioral health and substance use data
The governance challenge reaches its greatest complexity in behavioral health and substance use disorder data, precisely the data that is most consequential for the highest-risk patients and most restricted in exchange. 42 CFR Part 2 has historically imposed stricter consent requirements than standard HIPAA, creating a regulatory environment in which substance use disorder data was effectively walled off from clinical exchange. Regulatory changes in 2024 brought 42 CFR Part 2 into closer alignment with HIPAA, expanding permissible disclosures for treatment, payment and operations purposes, but the practical impact is still working through implementation. State mental health privacy laws add another layer that any system serving a national health plan must navigate in real time.
Behavioral health network connectivity is one of the most significant remaining white spaces in the interoperability landscape. The organizations building governance-embedded exchange infrastructure for this domain are addressing a genuinely hard problem with large clinical and commercial stakes. Systems that can demonstrate embedded governance—an auditable, configurable, policy-enforcing delivery architecture—remove the primary adoption barrier for the most risk-sensitive participants in the exchange ecosystem. As a result, the governance layer is a competitive differentiator.
Behavioral health network connectivity is one of the most significant remaining white spaces in the interoperability landscape. The organizations building governance-embedded exchange infrastructure for this domain are addressing a genuinely hard problem with genuinely large clinical and commercial stakes.
The infrastructure stack and where value is being created
The transition from systems of record to systems of action is not a single technology shift. It is a layered set of capabilities, each building on the one beneath it. The map below traces those layers across the four eras of clinical data infrastructure and illustrates why the exchange and transport layer running through all of them only grows in strategic importance as the application layers above it become more sophisticated.
The clinical data infrastructure stack
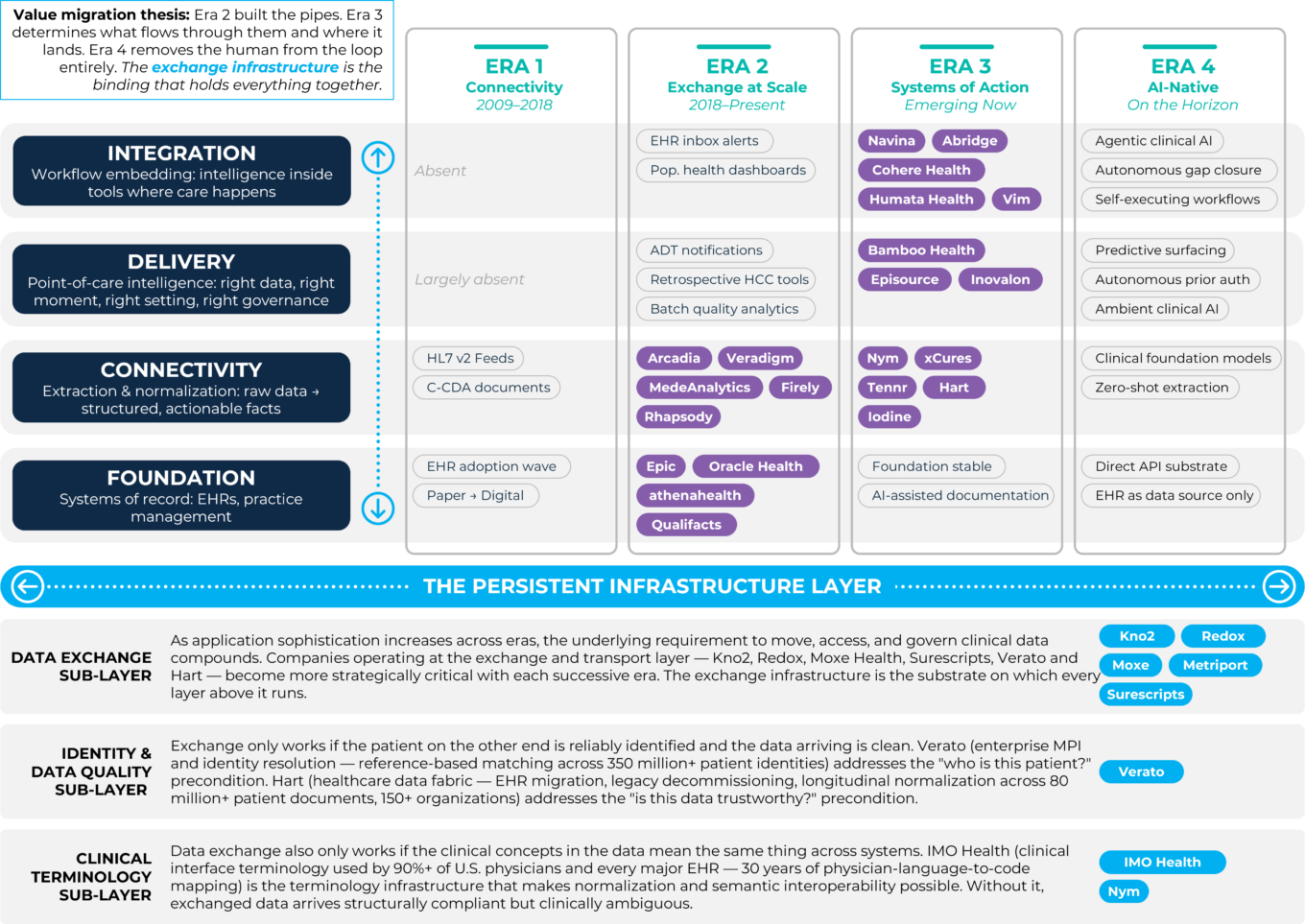
Source: First Analysis.
Where the opportunity is taking shape
The transition from systems of record to systems of action is generating a broad and heterogeneous opportunity landscape. The category looks meaningfully different depending on where in the stack and where in the care delivery ecosystem a company is positioned.
For health plans
Health plans, particularly Medicare Advantage plans operating in a compressed margin environment, are among the most motivated buyers in the systems-of-action category. The return on investment is quantifiable: HCC recapture rates translate directly to revenue. HEDIS improvement translates to star rating bonus eligibility, and prior authorization automation translates to administrative cost reduction. The challenge for plan technology buyers is distinguishing between vendors offering data access and vendors offering data delivery.
The following is a sampling of the capability areas where systems-of-action companies are creating value for health plans:
- real-time clinical data exchange platforms that surface HCC-relevant evidence prospectively rather than retrospectively
- prior authorization decision support tools that draw on live clinical data to accelerate utilization management decisions
- HEDIS gap closure platforms that reach diverse provider types
- dual eligible care coordination infrastructure that connects the fragmented stakeholder ecosystem around the most complex members
For providers and post-acute care settings
On the provider side, the most significant unmet need is in the care settings structurally excluded from the interoperability gains of the past decade. Home health agencies, skilled nursing facilities, behavioral health providers and community-based organizations need systems that can receive structured clinical context at admission, surface relevant information at the point of encounter, and contribute clinical data back into the shared record in a standardized form.
A sampling of companies building in this space
The exchange layer
The companies that move clinical data between systems (the exchange layer) have spent much of the past decade being treated as utilities: important, but largely interchangeable. That framing is increasingly wrong. As the application layers above the exchange infrastructure grow more sophisticated, the quality, reach and governance of the underlying pipes compound in strategic value. The exchange infrastructure is the substrate on which every successive application era runs.

Metriport’s open-source FHIR platform provides CommonWell and Carequality connectivity via APIs, allowing developers and healthcare organizations to build on top of the national exchange infrastructure without proprietary lock-in. The model is strategically important, because an open-source exchange layer lowers the barrier to building clinical data-enabled applications and creates a development ecosystem around interoperability infrastructure, which is ultimately how any network grows. Where other exchange platforms monetize network access as a product, Metriport is building toward a model in which the infrastructure itself becomes broadly available and value accrues at the application layer above it.

Moxe Health occupies a focused but structurally important position within the exchange layer. Rather than delivering data to providers, it specializes in payer-initiated clinical data retrieval, automating the collection of medical records for risk adjustment, quality measurement and prior authorization workflows. The demand signal is direct. Payers have been trying to reduce the cost and latency of clinical record retrieval for years, and the combination of TEFCA infrastructure maturation and CMS risk adjustment scrutiny has made automated, auditable retrieval infrastructure progressively more essential.

Kno2, a First Analysis venture capital portfolio company, has built its position in the part of the exchange landscape that most others avoid: treatment-domain clinical data flowing to and from post-acute, out-of-hospital, and behavioral health settings that sit outside the dominant EHR footprint. Skilled nursing facilities, home health agencies, hospice providers and community-based organizations serve patients who are often the most clinically complex and whose records are the most likely to be missing when care decisions are made upstream. The company connects more than 15,000 endpoints across this continuum, with document exchange infrastructure built specifically for the treatment-domain use cases that acute-care-focused or payer-facing networks were not designed to handle. Its participation in TEFCA’s Qualified Health Information Network framework positions it to benefit as the national data-sharing infrastructure matures. The significance of its partnership with Clover Health extends beyond a single customer relationship: placing a Medicare Advantage payer directly on top of Kno2’s exchange network is a directional signal about where payer data strategy is heading. As payers move from retrospective claims analysis toward real-time clinical data acquisition across the full continuum, including the post-acute and community-based settings that claims data describes incompletely, exchange infrastructure built for those settings becomes disproportionately strategic.

Redox has built its position as the integration translation layer connecting the digital health and clinical application ecosystem to the acute-care EHR environment, supporting HL7 v2, FHIR, and proprietary EHR APIs across more than 12,000 healthcare organizations. The proliferation of clinical applications needing EHR connectivity has expanded Redox’s addressable surface. There are more ambient documentation tools, care management platforms and clinical decision support applications that need to connect to more EHR environments than there were five years ago, and the complexity of managing those connections has not decreased.

Surescripts operates at a scale that sets it apart from every pure-play exchange infrastructure company in the market, having processed more than 30 billion transactions in 2025 across e-prescribing, benefit information, prior authorization and medication history. Its Real-Time Prescription Benefit product, used more than one billion times by prescribers last year, delivers point-of-care formulary and cost information directly into the prescribing workflow in a way that measurably changes what gets prescribed. For the interoperability thesis, what Surescripts illustrates most clearly is the durable value of load-bearing exchange infrastructure. When clinical workflows have been rebuilt on top of a network over two decades, that network cannot be displaced quickly or cheaply by anything that is not already embedded at the same depth.
The connective layer
The connective layer begins with identity and ends with intelligence. Raw information arriving from disparate sources—HL7 v2 messages, C-CDA documents, FHIR bundles of variable completeness—must be normalized, deduplicated and translated into structured facts that can be queried before it can inform a downstream decision. But before normalization can happen reliably, you need to know the records you are receiving belong to the right patient.
Arcadia has built a health data aggregation and analytics platform spanning payer and provider organizations. It normalizes EHR, claims, lab, and admission, discharge and transfer sources into a unified longitudinal patient record used by health systems managing value-based contracts and payers monitoring network performance. Its strength is in clinical data normalization for the provider-side value-based-care environment, where the depth of the normalization work underneath determines the quality of the care gap, risk and quality intelligence above.

Mede Analytics approaches the same analytics problem from the payer and employer side, serving health plans, third-party administrators, and self-insured employers managing total medical spend, utilization trends, and benefit design optimization. Where Arcadia is normalizing toward a longitudinal clinical record, Mede Analytics is normalizing toward a total cost-of-care view. This distinction reflects how the same exchange infrastructure creates value differently depending on who is doing the asking.

Hart operates a healthcare data fabric platform that spans the full clinical data life cycle: acquiring records from EHRs, ancillary systems, and devices across all major standards; normalizing and validating them into a persistent, longitudinal data foundation; and streaming structured data to analytics platforms, AI models, and population health tools without re-engineering or manual intervention. The platform has unified more than 80 million patient documents across more than 150 healthcare organizations. Its particular strength in EHR migration and legacy system decommissioning addresses one of the most acute and underserved problems in health system IT: the accumulation of fragmented historical data across multiple legacy EHR environments following years of mergers, acquisitions and system changes. Where interface engines handle message translation at the point of exchange, Hart builds a persistent, validated data layer that decouples downstream applications from the fragility of point-to-point integration. This is increasingly the architecture that large health systems and payers need as their data activation ambitions outgrow their current infrastructure.

IMO Health (formerly Intelligent Medical Objects) addresses the terminology layer of the normalization problem by ensuring that the same clinical concept means the same thing regardless of which EHR system, coder or clinical workflow generated it. Its clinical intelligence platform maps clinical documentation to standardized terminologies such as the International Classification of Diseases (ICD), Systematized Nomenclature of Medicine, Logical Observation Identifiers Names and Codes, and RxNorm (normalized names for clinical drugs), enabling structured data from disparate sources to be compared, aggregated and acted upon consistently. In the context of data exchange, IMO sits at the intersection of syntax and semantics: a record that has been structurally normalized by an interface engine or data fabric still may not be clinically interoperable if the underlying terminology is inconsistent. That is the problem IMO was built to solve, and its relevance compounds as the volume of exchanged clinical data increases.

Nym Health is applying AI-native logic to the coding layer itself, converting clinical documentation directly into ICD and Current Procedural Terminology (CPT) codes without human coder review. This is a zero-touch model that eliminates the per-encounter labor cost that has historically governed medical coding.

Iodine (Waystar) addresses the same documentation layer from the clinical documentation improvement direction, using clinical AI to surface gaps in clinical documentation that affect coding accuracy and downstream revenue cycle performance. Its acquisition by Waystar, one of the larger revenue cycle management platforms in the market, reflects the consolidation dynamic at work across this segment. Together with IMO Health’s terminology standardization capabilities, these three companies occupy adjacent positions in the clinical intelligence and coding layer of the normalization stack and represent a cohort of strategically motivated consolidators as the interoperability infrastructure matures, data volumes scale and the economic value of converting unstructured clinical information into structured, actionable facts becomes impossible to ignore.

Rhapsody is one of the most broadly deployed clinical integration and normalization engines in the market, with installations across health systems, payer organizations and health information exchanges. Its core strength is HL7 v2 message translation—converting the legacy clinical message infrastructure that most health systems still run into formats that modern analytics and application platforms can consume. The unglamorous nature of this work masks its strategic importance: an AI-powered population health platform or a prospective risk-capture tool is only as good as the normalization infrastructure beneath it.

Tennr has built AI-powered document intelligence for healthcare referrals and intake workflows, processing the faxes, referral packets and prior authorization documents that still govern how patients move between providers in most health systems. Its platform extracts structured clinical data from unstructured intake documents using AI, reducing the manual review that delays referral acceptance and downstream care coordination. In the context of the interoperability stack, Tennr addresses the entry point where structured exchange most commonly breaks down: when the documents entering the system were never structured to begin with.

Veradigm, the data and analytics business formerly associated with Allscripts, operates one of the largest real-world clinical data networks in the ambulatory physician practice market. The Veradigm Network’s scale reflects decades of EHR penetration in physician practice settings, creating a data asset that is difficult to assemble from scratch and that sits in the ambulatory, community-based, specialist segment of the care continuum where Epic and Oracle Health are not always the dominant systems. For life sciences companies, payers, and population health platforms trying to understand real-world care patterns outside the hospital, Veradigm occupies a connective tissue role whose value is a direct function of its breadth.

Verato addresses a prerequisite that every other exchange use case depends on: knowing that the records arriving for a given patient actually belong to that patient. Its master patient indexing (MPI) and identity resolution platform applies probabilistic matching to resolve patient identities across disparate source systems including clinical, claims and administrative, reducing the duplicate records and mismatches that corrupt exchange value at scale. For TEFCA networks, health information exchanges and health systems processing high volumes of inbound clinical records, the identity resolution layer is not optional infrastructure. A normalized record matched to the wrong patient creates clinical risk, and a data liquidity network without trusted identity is a liability as much as an asset.
The delivery layer
The delivery layer is where the interoperability infrastructure earns its return. Data that has been moved, normalized and structured still needs to land somewhere that changes a decision. The thesis underpinning the third era of clinical data exchange is that the right clinical fact, such as a risk flag, a care gap, a behavioral health signal or a prospective HCC code, can reach the right clinician or care team at the moment it remains actionable. The companies operating in this layer are not primarily in the data business. They are in the behavior change business, using data infrastructure as the enabler.

Bamboo Health has built a real-time care event notification network with particular reach into the behavioral health settings that most admission, discharge and transfer notification services do not cover. Its connections to crisis stabilization, detox and substance use disorder treatment facilities give it access to a category of clinical signal, behavioral health encounters, that is among the highest-value triggers for downstream care coordination and among the least likely to be captured by standard notification infrastructure. For payers and care management organizations managing high-complexity members, closing this gap is the central challenge.

Episource (Optum) operates in the Medicare Advantage risk adjustment market, focusing on prospective HCC category capture. It delivers risk-relevant clinical context to providers before and during the encounter, rather than retrieving charts retrospectively. The economics are direct. Retrospective chart retrieval is expensive, often incomplete, and arrives too late to change the clinical documentation that drives risk-adjusted revenue. Episource’s model uses exchange infrastructure to bring the right clinical context to the right moment, improving documentation accuracy and clinical completeness. As CMS intensifies scrutiny on Medicare Advantage risk adjustment practices, Episource makes the underlying process more auditable and defensible. Its position within the Optum ecosystem gives it distribution advantages that few independent vendors can match, though the prospective risk capture model it pioneered is now being pursued across the market by a range of independent and payer-affiliated competitors.

Inovalon has built one of the largest healthcare data and analytics platforms in the market, with capabilities spanning HEDIS quality measurement, care gap identification, risk adjustment analytics and clinical data exchange across payer and provider organizations. The platform’s approach to HEDIS gap closure—routing clinical data through exchange connections to diverse provider types before measurement windows close—illustrates the delivery layer thesis directly. The value is not in identifying the gap, which retrospective analytics have done for years, but rather in closing the gap at a point where a clinical action can still occur.
The integration layer
The integration layer is the part of the stack that clinicians actually touch, the point where an exchange network, a normalization engine, and a delivery mechanism either surface a useful clinical output or disappear as unrealized potential. AI-powered patient summaries at the point of documentation, ambient tools capturing a clinician’s words, and care gap alerts appearing inside the EHR are all visible expressions of infrastructure that had to work correctly before any of it could appear. Three companies illustrate the third era’s integration opportunity from different angles.

Abridge has built ambient clinical documentation technology that converts natural conversation between clinicians and patients into structured clinical notes, reducing the documentation burden that ranks among the most consistently cited drivers of physician burnout. The interoperability implication is underappreciated. Ambient documentation improves the quality and specificity of structured data at the point of generation. Normalization engines, risk adjustment platforms, quality measurement systems, and payer analytics all start from a better position when the source data is more complete and more accurately coded. Abridge is positioned at the very beginning of the clinical data life cycle, and what it captures has compounding effects on every layer that follows.

Navina surfaces AI-assisted clinical decision support inside the EHR documentation workflow, aggregating patient records from multiple sources and translating them into a longitudinal patient summary available at the moment of the clinical encounter. For Medicare Advantage plans and their provider partners, the value proposition is to surface prospective risk conditions during the visit, grounded in the patient’s actual clinical history, rather than through retrospective administrative review after the encounter window has closed. The physician receives synthesized clinical context rather than unsorted records, which changes both the documentation behavior and the clinical completeness of what gets captured.

Vim takes the integration opportunity from the payer’s direction rather than the provider’s. Its platform embeds health plan clinical intelligence directly inside the EHR workflow, surfacing care gap alerts, prior authorization guidance, and care coordination prompts to providers at the point of care without requiring the clinician to navigate outside the environment they are already using. The bidirectional connectivity between payer and provider at the workflow level represents a structural shift in how plan-provider relationships operate. Rather than retrospective reporting and administrative friction, Vim enables real-time, workflow-embedded dialogue. For Medicare Advantage plans trying to close HEDIS gaps, improve prospective risk documentation, and reduce prior authorization friction simultaneously, the EHR-embedded channel is qualitatively different from any outreach mechanism that sits outside the clinical workflow.
Evaluating the category
For health plan and health system executives navigating this market, the marketing language has become sufficiently homogenized that meaningful differentiation requires looking past the surface claims. A handful of dimensions tend to separate vendors doing something real from those selling a vision.
Network breadth versus depth. How many connections does the exchange platform have, and how complete and current is the data at each connection? A network with 10,000 provider connections delivering 30-day-old document snapshots is a fundamentally different product from one with 4,000 connections delivering real-time discrete FHIR resources. The numerator matters considerably less than what it actually delivers.
Normalization quality. Does the platform deliver raw HL7 or FHIR feeds, or structured, normalized clinical data elements? A raw feed requires downstream processing; a normalized discrete element can drive action. Understanding where in the data pipeline a vendor’s product ends and where the customer’s implementation work begins is critical to realistic deployment planning.
Latency and trigger architecture. For prior authorization, care transitions and point-of-care decision support, latency is a key consideration. A system that delivers clinical context 72 hours after an admission-discharge-transfer event is not a system of action; it is a delayed system of record. How a vendor’s platform triggers data delivery, and what the realistic end-to-end latency looks like in production, tells you a great deal about where it sits in the stack.
Care setting coverage. Does the network reach the care settings where the highest-cost members receive care? A platform with deep hospital and large physician group connectivity but limited post-acute and behavioral health reach may be solving 60% of the data gap while leaving the hardest 40% unaddressed.
Governance architecture. Is treatment, payment, and healthcare operations compliance embedded in the delivery layer, or is it a policy wrapper around a generic data pipe? An auditable, configurable governance architecture is not just a legal requirement, but also an adoption enabler for the provider organizations that need to participate in the network.
The transition underway
The market dynamics shaping this category follow a logic that is by now familiar from other infrastructure transitions, even if the specific mechanics are new. The following are a few observations about how we expect this to develop.
The opportunity is at the edges, not the center. Major health systems and large commercial payers have workable solutions for their core use cases. The more significant unmet need—and the more interesting near-term opportunity—is at the edges: behavioral health providers, post-acute settings, dual eligible care coordination and home-based care. These are the settings with the least infrastructure, the most complex patients and the most to gain. They are also the settings that have been structurally excluded from the interoperability gains of the past decade.
Governance architecture is a real competitive moat. A platform that can navigate 42 CFR Part 2, state mental health privacy laws and TPO-compliant HIPAA exchange in real time has built something genuinely difficult to replicate. The switching costs are real, and they compound with each new care setting the platform reaches.
AI is a tailwind, not a threat. Every AI initiative at a health plan that runs into its data pipelines as the binding constraint is a potential customer for the action layer. Autonomous agents need clean, trusted, governed data at machine speed. The companies building that substrate now are positioning for a demand curve that AI adoption is accelerating materially.
The network-building window is open now. The organizations that achieve critical mass in terms of provider connections, data volume and payer relationships will become increasingly difficult to displace. The window for building competitively differentiated networks is open now but will not remain open indefinitely.
The home health nurse at the kitchen table on day one of a care episode should not have to work from a 47-page PDF. The skilled nursing facility admission team should not have to call the discharging hospital to find out what medications were changed. The behavioral health provider should not have to ask the patient to reconstruct their medical history because the clinical record never arrived.
These are not aspirational scenarios. They are what systems of action, properly built, can deliver today. In the early deployments, this infrastructure is being proven. Technology is no longer the primary constraint. The needed exchange standards exist. The regulatory framework is more enabling than it has ever been. And the demand signal, driven by AI adoption and margin compression in Medicare Advantage, has never been stronger.
The technology constraints that defined the first two eras — getting data into systems, then getting systems connected — are largely resolved. What remains is a delivery problem. The demand signal is real. The regulatory environment is more enabling than it has ever been, and the AI wave is pulling the timeline forward. The companies building the action layer now are not early — they are on time.
Healthcare tech indexes continue to lag broad market
The First Analysis Healthcare Technology Index finished the one-year period ended May 4 down 31.2% overall, with the payer technology subset down 34.8% and the provider technology subset down 30.6%. Over the same period, the S&P 500 gained 27.4%, and the Nasdaq gained 40.5%.
Of the 18 First Analysis healthcare technology companies that were publicly traded at the beginning of the period, the stock prices of only three were up over the period. CareCloud (CCLD) increased by the most, 54%. The next two largest gainers were Omnicell (OMCL), up 39%, and Veradigm (MDRX), up 10%. Of the 15 stocks that declined, 10 declined by 20% or more. GoHealth (GOCO) declined the most, 88%, followed by Definitive Healthcare (DH), which declined 63.7%. Doximity (DOCS), which was almost a third of the index’s total market capitalization at the beginning of the period, accounted for over half the index’s decline due to a 58% decline in its stock price.
Healthcare technology public comparables* ($ in millions)
| Company ($ in millions) | LTM revenue |
Rev growth ’25A–’26E |
Rev growth ’26E–’27E |
LTM gross margin |
LTM EBITDA margin |
EV/rev ’26E |
EV/rev ’27E |
EV/EBITDA¹ ’26E |
EV/EBITDA¹ ’27E |
|---|---|---|---|---|---|---|---|---|---|
| Payer technology | |||||||||
| American Well (AMWL) | $237.4 | (20.0%) | 4.1% | 53.4% | (19.9%) | NMF | NMF | 2.7x | 7.8x |
| eHealth (EHTH) | $554.0 | (22.8%) | 5.6% | 100.0% | 12.7% | 1.16x | 1.10x | 7.9x | 7.1x |
| EverQuote (EVER) | $716.7 | 12.7% | 11.3% | 97.5% | 10.4% | 0.45x | 0.40x | 3.0x | 2.6x |
| Evolent Health (EVH) | $1,876.2 | 32.8% | 15.4% | 21.3% | 4.7% | 0.52x | 0.45x | 10.5x | 7.9x |
| Omada Health (OMDA) | $260.2 | 22.6% | 19.9% | 65.7% | (2.5%) | 2.23x | 1.86x | NMF | 36.3x |
| TruBridge (TBRG) | $346.8 | 2.2% | 4.7% | 53.0% | 11.1% | 1.46x | 1.39x | 6.8x | 6.3x |
| Veradigm (MDRX) | $588.0 | (1.0%) | 1.7% | 52.5% | 8.8% | 1.02x | 1.00x | 7.0x | 6.2x |
| Mean | $654.2 | 3.8% | 9.0% | 63.3% | 3.6% | 1.14x | 1.03x | 6.3x | 10.6x |
| Median | $554.0 | 2.2% | 5.6% | 53.4% | 8.8% | 1.09x | 1.05x | 6.9x | 7.1x |
| Provider technology | |||||||||
| CareCloud (MTBC) | $120.5 | 8.9% | 8.3% | 46.5% | 13.6% | 0.95x | 0.88x | 4.1x | 3.6x |
| Definitive Healthcare (DH) | $241.5 | (7.4%) | 0.7% | 84.3% | 14.7% | 0.89x | 0.88x | 3.6x | 3.5x |
| Doximity (DOCS) | $637.8 | 6.2% | 7.8% | 89.7% | 38.5% | 5.72x | 5.30x | 10.8x | 9.7x |
| GoHealth (GOCO) | $361.8 | (28.4%) | NMF | 73.4% | (22.1%) | 2.37x | 1.21x | 49.7x | 13.1x |
| GoodRx (GDRX) | $796.9 | (4.0%) | 5.7% | 92.8% | 15.3% | 1.49x | 1.41x | 4.8x | 4.5x |
| Health Catalyst (HCAT) | $311.1 | (9.9%) | 1.6% | 49.7% | (1.7%) | 0.68x | 0.67x | 5.4x | 5.2x |
| HealthEquity (HQY) | $1,313.4 | 7.5% | 8.2% | 69.5% | 36.7% | 5.40x | 4.99x | 12.2x | 10.9x |
| HealthStream (HSTM) | $311.8 | 7.3% | 5.1% | 64.9% | 13.5% | 1.75x | 1.66x | 7.6x | 7.0x |
| Maximus (MMS) | $5,373.6 | 0.1% | 5.6% | 25.1% | 13.0% | 0.94x | 0.89x | 6.6x | 6.4x |
| Omnicell (OMCL) | $1,225.1 | 5.3% | 5.5% | 43.9% | 5.9% | 1.54x | 1.47x | 11.8x | 10.6x |
| Phreesia (PHR) | $480.6 | 7.3% | 5.1% | 67.9% | 4.3% | 1.20x | 1.14x | 4.8x | 4.3x |
| Teladoc Health (TDOC) | $2,514.5 | (0.9%) | 1.4% | 69.3% | 1.9% | 0.59x | 0.58x | 5.3x | 5.0x |
| Mean | $1,140.7 | (0.7%) | 5.0% | 64.8% | 11.1% | 1.96x | 1.76x | 10.6x | 7.0x |
| Median | $559.2 | 2.7% | 5.5% | 68.6% | 13.3% | 1.34x | 1.18x | 6.0x | 5.8x |
Source: Capital IQ, First Analysis.
Notes: Public comparable company data shown above is as of May 4, 2026. (1) EBITDA multiples less than 0 and greater than 50 labeled “not meaningful” (NMF). LTM = last 12 months. EBITDA = earnings before interest, taxes, depreciation and amortization.
The indexes’ enterprise value multiples of trailing 12-month revenue as of May 4 were 0.9 for the payer technology subset and 1.7 for the provider technology subset. Regarding forward multiples, the average and median enterprise value multiples of 2026 estimated revenue were both 1.1 for the payer technology subset and 2.0 and 1.3 for the provider technology subset. The average and median enterprise value multiples of 2027 projected revenue were 1.0 and 1.1 for the payer technology subset and 1.8 and 1.2 for the provider technology subset. In the payer technology subset, Omada Health (OMDA) continued to trade at the highest multiple of 2026 estimated revenue (now 2.2), while Doximity (DOCS) led the provider technology subset at 5.7.
The overall growth outlook was almost unchanged from our last report in early April. The average 2026 estimated revenue growth rate is 3.8% for the payer technology subset and -0.7% for the provider technology subset. Average revenue growth for 2027 is expected to accelerate for both groups, to 9.0% for payer technology and to 5.0% for provider technology.
First Analysis Healthcare Technology Index 1-year performance
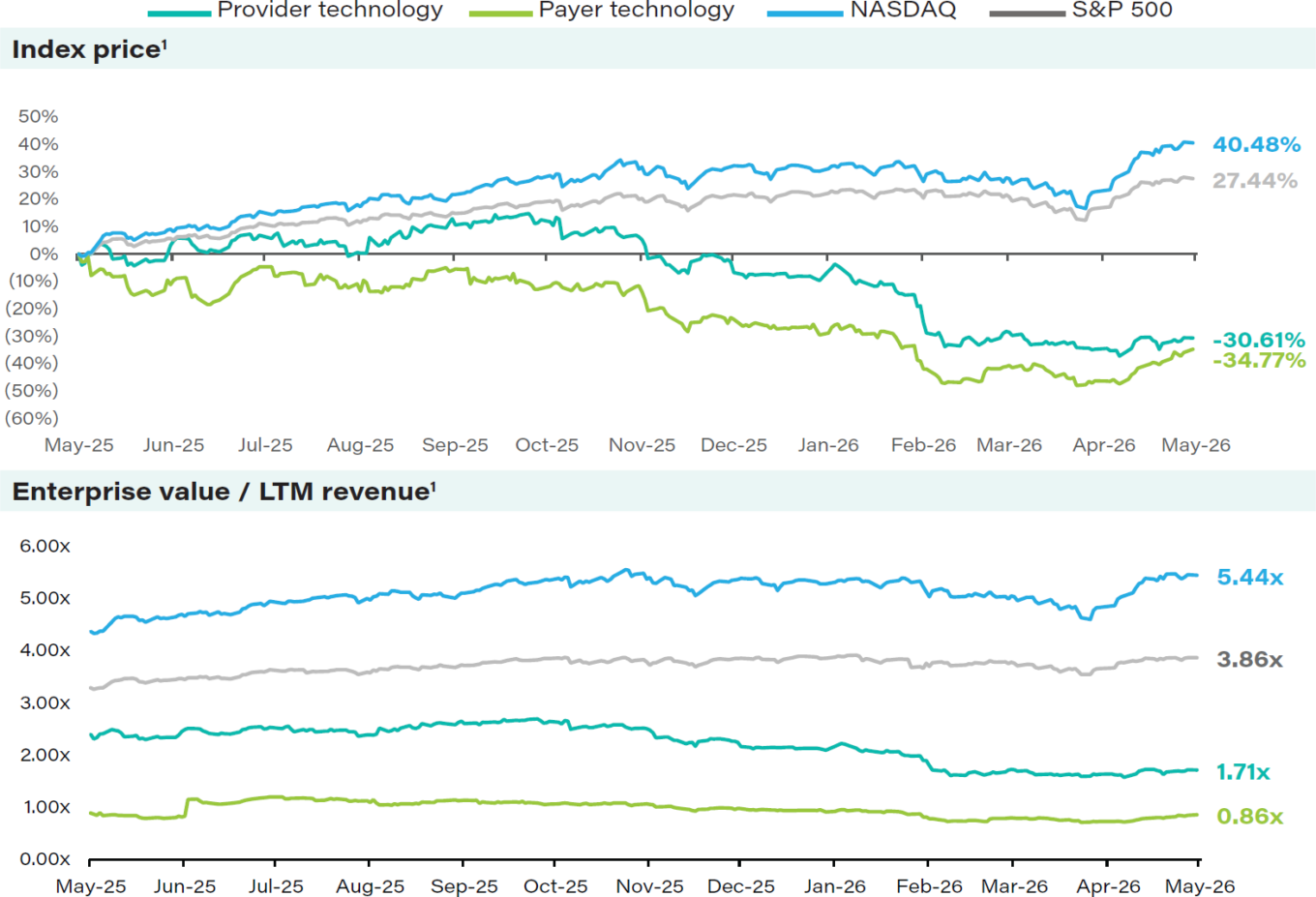
Source: Capital IQ.
Notes: (1) Index performance is based on market cap weighted constituents. For the period from May 5, 2025, through May 4, 2026.
Healthcare tech M&A: Notable transactions include Knack RCM, EqualizeRCM, Bonsai Health
We highlight three recent acquisitions that reflect growing strategic focus on AI-native platforms purpose-built to absorb high-volume administrative work across revenue cycle management and patient engagement, areas where healthcare providers face persistent staffing pressure and rising operating costs.
On May 4, Carlyle announced it acquired Knack RCM and EqualizeRCM in concurrent transactions and is combining the two businesses to create an AI-native global revenue cycle management (RCM) platform. Transaction terms were not disclosed. Knack RCM and EqualizeRCM both provide healthcare revenue cycle management services to provider organizations across the United States, including coding, billing, claims management, denial management and collections. The combined companies represent a platform built around large language models and automation rather than retrofitted onto legacy systems. Carlyle’s investment comes as healthcare providers face persistent labor shortages, rising denial rates and growing complexity in payer mix, conditions that have driven sustained demand for outsourced RCM with embedded AI to lift productivity and yield.
On April 20, ModMed announced it acquired Bonsai Health, an agentic AI patient engagement platform. Transaction terms were not disclosed. Bonsai Health provides agentic AI applications that automate patient-facing workflows including scheduling, intake, reminders, follow-up and routine clinical communications. ModMed develops specialty-specific electronic health record, practice management and revenue cycle solutions. Embedding Bonsai’s agentic AI directly into ModMed’s specialty platforms is intended to extend the AI-Powered Practice strategy ModMed has emphasized, automating high-volume, low-complexity patient interactions so clinicians and staff can focus on care delivery.
Bonsai is an AI-powered platform built to improve patient outcomes, reduce staff workload, and keep providers’ schedules full
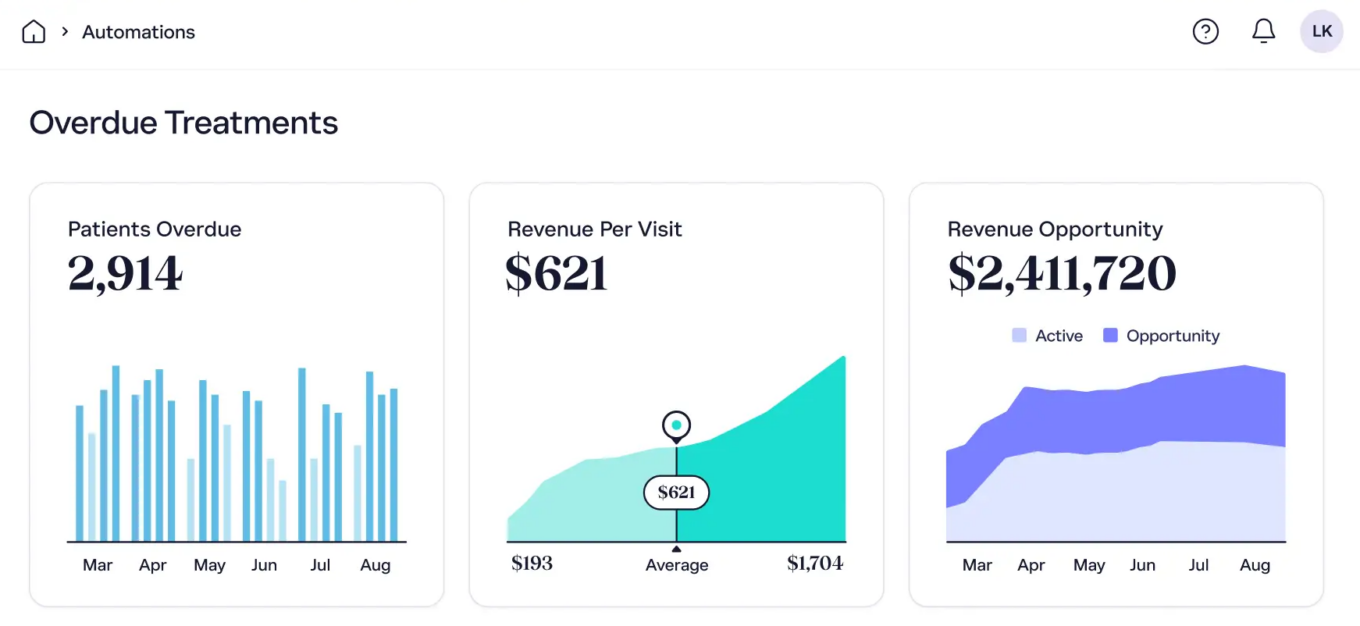
Source: Bonsai Health.
Select recent M&A transactions (sorted by date of announcement, $ in millions)
| Date | Target | Target business description |
Buyer | Enterprise value ($ in millions) |
Enterprise value/rev ($ in millions) |
|---|---|---|---|---|---|
| 5/4/2026 | EqualizeRCM | Healthcare revenue cycle management provider | Carlyle | Undisclosed | Undisclosed |
| 5/4/2026 | Knack RCM | Healthcare revenue cycle management provider | Carlyle | Undisclosed | Undisclosed |
| 4/22/2026 | Team Recovery Technologies | Patient engagement software provider for behavioral health treatment | Kipu Health | Undisclosed | Undisclosed |
| 4/20/2026 | Bonsai Health | Agentic AI applications that automate patient-facing workflows including scheduling, intake, reminders, follow-up and routine clinical communications | ModMed | Undisclosed | Undisclosed |
| 4/16/2026 | ProModRx | Software to speed patient access to prescription medications | D2 Solutions | Undisclosed | Undisclosed |
| 4/16/2026 | Tria Health | Provider of pharmacist-led patient support and dispensing solutions for self-insured employers | Stellus Rx | Undisclosed | Undisclosed |
Source: Capital IQ, First Analysis.
Healthcare tech private placements: Notable transactions include Enzo Health, Luminai
We highlight two recent private placements that reflect growing investor appetite for AI-native platforms that absorb high-volume, repetitive administrative work in home-based care and hospital operations, areas where legacy software and human coordination layers have struggled to keep pace with demand.
On May 4, Enzo Health announced a $20 million Series A funding led by N47 with participation from Gradient, Tandem Ventures, Rigby Watts, Lionel Partners and Soma. The round brings total funding to $26 million. Enzo Health provides an AI-native platform for home-based care agencies that automates referral intake, clinical documentation (including OASIS charting), scheduling, billing and quality assurance. The platform is built for home health, hospice and skilled nursing settings, where most agencies still operate on legacy software designed in the fax-and-paperwork era. Enzo was founded in 2024, and the agencies using its platform collectively support more than 500,000 patients each year. Clinician turnover among home health professionals exceeds 80% within the first 100 days at many agencies, a problem driven largely by administrative burden that Enzo’s AI automation is designed to absorb. The financing will support continued platform development and expansion into skilled nursing and hospice.
Enzo Health’s AI-native platform for home-based care agencies automates referral intake, clinical documentation, scheduling, billing and quality assurance
Source: Enzo Health.
On April 9, Luminai announced a $38 million Series B funding led by Peak XV Partners with participation from Define Ventures, General Catalyst, Y Combinator and Scribble Ventures, alongside an announced partnership with Cleveland Clinic. The round brings total funding to $60 million. Luminai provides an AI agent platform that automates operational workflows across health system back offices, processing unstructured inputs such as faxed referrals, EHR messages, payer policies and contracts and orchestrating downstream actions across systems of record. The platform encodes institutional logic into versioned, auditable workflows and routes exceptions to human operators with full context, so judgment improves over time as the system learns from each handoff. Luminai’s platform supports more than 12 million workflow automations, with an average time-to-value of 48 days for new use cases. The Cleveland Clinic deployment begins with referral routing across the system’s 23 hospitals, classifying and directing incoming faxed referrals across thousands of possible destinations using the same operational logic a trained staff member would apply. The financing will support expansion of Luminai’s engineering teams and acceleration of new use-case rollouts at health systems.
Luminai overview

Source: Luminai.
Select recent private placements (sorted by date of announcement, $ in millions)
| Date | Company | Business description |
Investors | Raise type | Amount raised |
Total amount raised |
|---|---|---|---|---|---|---|
| 5/4/2026 | Enzo Health | Automates documentation, coding, intake and quality assurance processes for home health agencies | N47; Gradient Ventures; Tandem Ventures; Rigby Watts; Soma; Lionel Partners | Series A | $20.0 | $26.0 |
| 4/27/2026 | TriFetch | Automation platform built for independent clinics and multi-specialty groups, automating the workflows that consume staff time such as patient calls and scheduling, referral processing, and prior authorizations | Nexus Venture Partners | Pre-Seed | $1.9 | $1.9 |
| 4/22/2026 | Courier Health | Patient experience management company | Oak HC/FT; Norwest Venture Partners; Work-Bench | Series B | $50.0 | $70.5 |
| 4/17/2026 | Joyful Health | Revenue recovery platform for healthcare providers | CRV; XYZ Venture Capital; Designer Fund; Inflect Health; Go Global Ventures | Series A | $17.0 | $17.0 |
| 4/16/2026 | Ethermed | Prior authorization and healthcare workflow automation company | Enfield Capital Partners; Blue Marlin Partners; Jumpstart Ventures; Healthliant Ventures; Gaingels | Series A | $8.5 | $8.5 |
| 4/15/2026 | Keebler Health | Risk adjustment platform to process unstructured clinical documentation for providers and payers | AngelList; Everywhere Ventures; Flare Capital; Freestyle Capital; Hustle Fund; MBX Capital; NC Tweener Fund; New Stack Ventures; Sands Capital; Tau Ventures; Underdog Labs | Series A | $16.0 | $22.0 |
| 4/9/2026 | Luminai | Healthcare automation platform that streamlines administrative operations for large health systems by automating complex, manual workflows such as referral intake, patient registration and claims management | Peak XV Partners; Define Ventures; General Catalyst; Y Combinator; Scribble Ventures | Series B | $38.0 | $60.0 |
| 4/6/2026 | Insight Health | Automates routine clinical tasks to streamline healthcare operations | Standard Capital; Pear VC; Kindred Ventures; Eudemian; ElevenLabs | Series A | $11.0 | $11.0 |
Source: Capital IQ, First Analysis.

Request full report
To access the full report, please provide your contact information in the form below. Thank you for your interest in First Analysis research.
